Hamstring tears are among the most common injury in sports, accounting for 15% of AFL injuries and 12% of soccer injuries. Generally speaking one in every five or six injuries sustained during sport is a hamstring tear. They are most often associated with maximal sprinting, acceleration or kicking. Unfortunately, up to a third of sustained hamstring injuries recur with greater severity. So as you can imagine it’s really important to get appropriate rehabilitation and care to not only get you back to sport and life sooner, but also reduce your risk of re-injury!
Mechanism of Injury
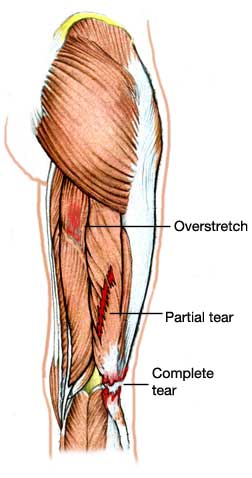
Type 1 Hamstring Tears are more common and occur during high speed running, often injuring the biceps femoris muscle. The increased demands at the end of the swing phase of sprinting requires the hamstring to work hard “eccentrically” to decelerate the swinging leg in preparation for foot strike and can lead to a tear.
The less common type 2 injuries occur during extensive lengthening of the hamstrings at variable speeds during a kicking motion (e.g. Kicking, ballet, gymnastics). The overstretching injury typically involves the semimembranosus and often requires an extended rehabilitation.


A third mechanism involves the high-power propulsion stage of acceleration. The combination of active hamstring contraction with trunk flexion that occurs during acceleration generates a high workload of the hamstring into a lengthening position that leads to muscle failure.
What happens when the muscle tears and how does it heal?
Below is a description of the different stages of healing and a guide to the indicated physiotherapy management during stage. Progression through these stages will vary between people. Progress is dependent on the severity of the injury, the specific muscle injured and the mechanism of the tear. Rehabilitation is also tailored to each individual, their activities and their goals. These stages will normally overlap and an ongoing strengthening program should be continued as the soft tissue continues to heal, even after discharge.
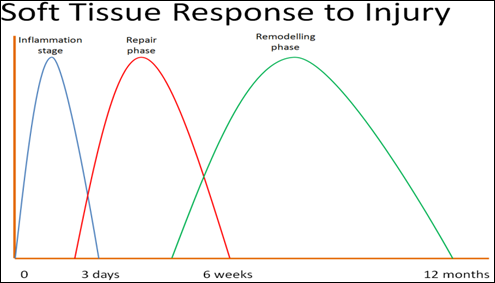
Phases of Soft Tissue Healing
- Acute Inflammatory Phase (0-96 hours)
- Repair Phase (2 days to 6 weeks)
- Remodelling Phase (4 weeks to 12 months)
These phases overlap as seen in the graph.
Stage 1: Inflammatory Stage
Chemicals are released into the damaged tissue producing pain, bleeding and an inflammatory response causing swelling.
What can you do to help healing?
Rest – avoid aggravating activities
Ice – apply ice to help reduce swelling and pain
Compression – Helps reduce swelling and provides support
Elevate – gravity can assist with removal of swelling & toxins
Physiotherapy treatment involves:
- Effleurage massage
- Gentle pain free mobilisations and movement exercises
- Ice, compression and elevation
- Stretches and strength training as indicated
Stage 2: Repair Stage
Blood starts to clot over the damaged tissue and scar tissue is formed. Scar tissue attempts to mesh the damaged ends of the torn ligament or muscle together. This does not form parallel fibres but a disorganised mesh. As stress and load is applied to the healing tissue, the tensile strength of the tissue increases.
Physiotherapy treatment involves:
- Scar tissue frictions
- Progression of movement and strengthening
- Soft tissue work on overactive compensatory muscles
- Normalising movement patterns and gait retraining,
- Address biomechanical flaws
Stage 3: Maturation/Remodelling
This stage involves the maturation and realignment of scar tissue into normal ligament or muscle tissue. The scar itself can start to assume the structure of pre-injured tissue. The initial severity of the injury and at what stage management commenced will largely influence the time taken for maturation
and whether complete remodelling will occur.
Physiotherapy treatment involves:
- Progression to global (whole body) strengthening, motor control and biomechanical retraining
- Progression of muscle conditioning
- More sports specific and dynamic exercises
- Running program
- Gradual return to sport and skill acquisition
- Patients should continue a rehabilitation program independently even after discharge in order to get the best outcome
What are the Risk Factors to tearing my hamstring?
- Previous hamstring or knee injury or pubic bone stress
- Kicking sports e.g. AFL, soccer, ballet
- Age
- Reduced hip range of motion
- Hamstring:Quadricep strength balance ratio
- Muscle fatigue (80% of injuries happen towards the end of a match)
- Poor Muscle activation patterns/weakness (weak core or gluteals)
How does physiotherapy help?
Once a hamstring tear occurs (no matter how severe), early physiotherapy is crucial to maximise the potential for favourable outcomes. The Physio will assess the severity of the injury, initiate acute care management of the hamstring tear and recommend appropriate treatment plan based on the patient’s goals. Treatment will focus on assisting muscle healing through manual therapy, address any biomechanical deficits found and include the prescription of a progressive exercise program made up of eccentric, concentric and neuromuscular strengthening, stretches and sport based functional exercises. This will also include an end stage running program, assisting a return to sprinting. Return to sport and full recovery is based upon objective measures to ensure muscle/strength imbalances, technique and biomechanics are corrected to help prevent re-injury.

What does the evidence say?
Hamstring tears have a high recurrence rate with Heirderscheit (2010) finding that almost a third of hamstring tears recur within the first year of returning to sport, often more severely. For this reason, a comprehensive, evidence-based rehabilitation program is essential to return to sport and prevent further injury. Askling et al (2014) showed rehabilitation programs that incorporate eccentric exercises improve both return to sport time and reduce the recurrence rate. Sidler et al (2013) also demonstrated that protocols incorporating agility, trunk stability, progressive running and eccentric strengthening achieved earlier return to sport and low re-injury rates. A physiotherapist is best placed to evaluate criteria for return to sport with pain on palpation (De Vos et al 2014), strength deficits of greater than 5% (Malliaropoulos et al 2011), insecurity with the active hamstring test (Askling et al) and poor single leg bridge test (Freckleton et al 2014) all being predictors an athlete is not safe to return to sport. This highlights the importance of completing hamstring rehabilitation with a Physiotherapist addressing various risk factors prior to returning to sport. Various injury characteristics can be used to predict recovery with high pain levels, bruising, proximal location, longer time to walk test and decreased passive straightening, predicting greater than 40 days to return to sport (Erickson et al 2017).
Can hamstring injuries be prevented?
As with any musculoskeletal injury, prevention is far superior to treatment. A pre-season screening can highlight any strength/length impairments or imbalances in the hamstring muscle group through specific testing. This screening can also assess biomechanics and other muscle groups that may lead to increased loading and eventual failure of the hamstring. Once assessed a Physiotherapist can then implement appropriate strength and exercise programs to prevent injury.
If you have injured yourself at sport or specifically sustain a hamstring tear book in for an assessment today:

Injury assessment & Treatment
- Get crystal clear about what’s causing your injury or pain
- Understand what activities you can do without delaying recovery and suffering consequences
- Find out what simple yet essential exercises can help you get amazing results
- Leave the session with the confidence of knowing exactly what to do to get symptom free and back to sport and living life without pain
Pre-screening Assessment for Sport & Gym
- Get a complete analysis of your movement and risk of injury
- Guidance regarding load management and how to avoid injury as a result
- Find out how to start training minimising your risk of injury
- Corrective exercises prescribed where needed
- Individualised program to achieve your goals