What is Sciatica?
Sciatica is a symptom rather than a specific diagnosis. Sciatica refers to symptoms that travel down the leg along the path of the sciatic nerve. These symptoms are often related to compression of the sciatic nerve, which can occur anywhere along its path from the lumbar spine, down through the hips and gluteal region and down the posterior leg through the hamstring, calf region and into the foot. These symptoms may include pain (usually described as “shooting” or “burning”), weakness, sensation loss, tingling, numbness and/or pins & needles.
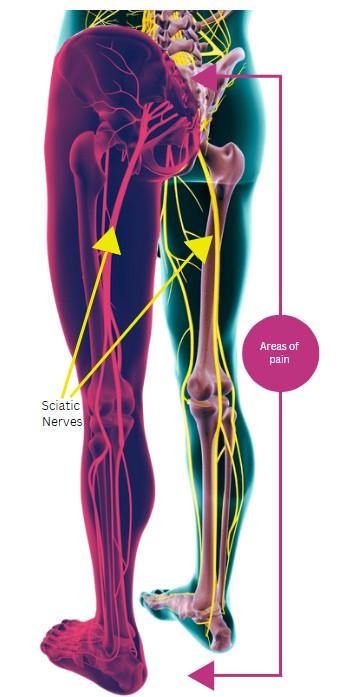
Anatomy
The Sciatic nerve originates from the nerve roots L4 to S3. The nerve travels posteriorly down the thigh where it becomes the tibial nerve as it passes between the femur and tibia. From there it branches into smaller nerves which supply the remainder of the leg and foot.
Due to this large area covered by the nerve, symptoms can occur anywhere from the gluteal area to the sole of the foot.
Causes of sciatica
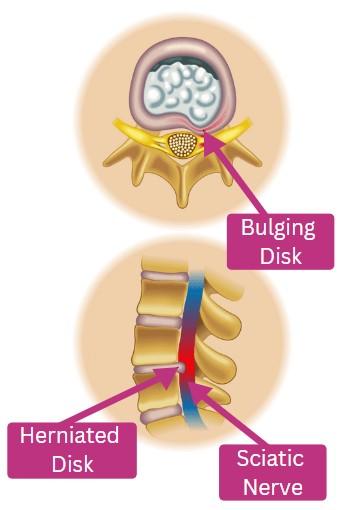
- Disc pathology
- Canal stenosis
- Piriformis syndrome
- Lumbar facet joint irritation/arthropathy
- Trigger point referrals
- Tumours
Treatment and Management
Treatment for sciatica will often consist of a period of non-operative treatment to help manage symptoms and restore function and well-being.
Physiotherapy is important as a first-line intervention for those suffering from sciatica. Physio’s will correctly classify and diagnose the cause of the symptoms, but also rule out any red flags or neurological conditions that require immediate surgical referral. Following a comprehensive assessment, our physios can help diagnose the source of pain and are also able to get an understanding of the underlying biomechanics and the compensations contributing to symptoms. Where needed, investigations like an x-ray, CT, and MRI can assist with this, and we will regularly liaise with the GP when these investigations are required. Imaging is not always necessary or helpful as physiotherapy treat the patient and not the scan (Brinjikji et al., 2015). Current global guidelines only recommend imaging in cases where serious pathology or radiculopathy is suspected, or if no improvement is seen after 4 weeks of Physiotherapy treatment.
Physio treatment of sciatica often involves a combination of manual therapy, a progressive exercise program, CBT, education, and advice. Alongside physiotherapy, GP-prescribed medication can be helpful to provide symptom relief and when patients lack progress through rehabilitation nerve root injections can also be beneficial at the GP’s discretion. Physio-prescribed manual therapy is particularly useful in the acute stage of recovery and can help to control symptoms by reducing muscle overactivity and improving joint mobility. Education regarding appropriate movements, posture, ergonomics, load management, and the dos and don’ts for the patient’s specific issue is essential to accelerated recovery. Exercise plays an incredibly important role. In the early stages of rehabilitation certain exercises aim to get our patients moving again and provide relief, whilst other exercises help restore muscle activation patterns including gluteal and core control. As progress is made, our physiotherapists will start to focus on strength, and progress motor control and endurance exercises. This progression through rehabilitation is essential to getting patients back to achieving their goals whether it be work/sport/life and preventing recurrences. Depending on the patient’s goals we will often guide this process and empower independence by taking our patients to the gym or leading them through a Clinical Pilates-based exercise program.

Pilates can improve general health, pain levels, sports functioning, flexibility and proprioception in individuals with chronic low back pain – Gladwell, 2006
When is surgery considered?
Surgery for sciatica is rarely used as the first line treatment. It is usually considered when it causes severe weakness, loss of bowel or bladder control, or when pain and symptoms are persistent or progressive after several methods of non-surgical treatment have been trialled. Certain conditions require surgical opinion immediately such as Cauda equina syndrome (pictured left), or when tumours or infection are present.
Evidence
Research into sciatica has consistently shown that conservative management, incorporating the key elements of education, advice, activity modification, manual therapy and a guided progressive exercise program to be the best practice treatmentas evident by the overview of the current guidelines (Oliveria et al., 2018, Owen et al., 2020). A variety of exercise programs have been shown effective with Wang et al. (2012) and Shamsi et al. (2015) demonstrating improvements in both pain and disability with either core specific or general low back exercise programs. Brukner et al. (2018) support the use of manual therapy in relieving symptoms, improving segmental mobility and relaxing muscle spasm. A study by Reddington et al. (2022) reported accelerated access to physiotherapy for those suffering with sciatica lead to a quicker recovery and avoided further physical and psychological deterioration, and thus we
encourage early referral or booking for those troubled by this condition.