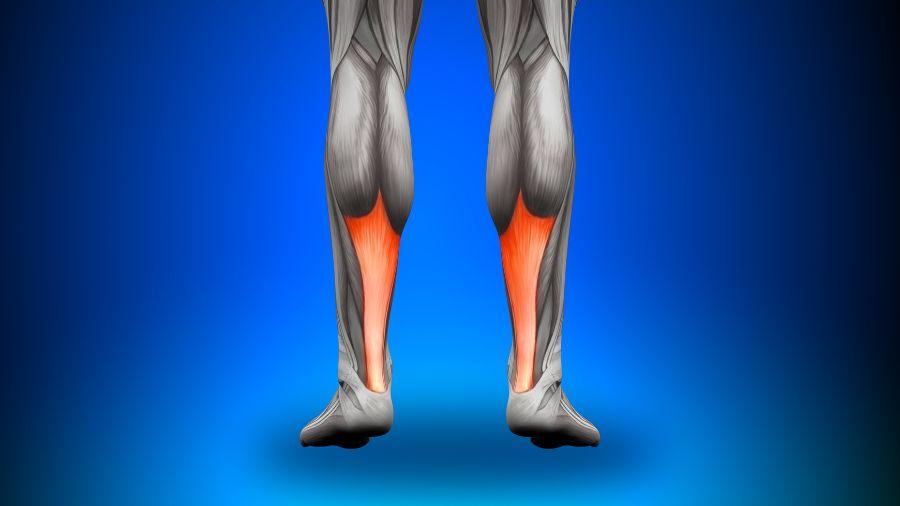
The Achilles tendon is the combined tendon of the gastrocnemius and soleus muscles and is the strongest tendon in the body.
It is prone to injury when exposed to activities involving repetitive high loads leading to pathological changes in the tendon due to this overuse and chronic stress. Repetitive high loads may include running, jumping, sudden acceleration or deceleration, or simply too much time on your feet in less supportive shoes.
Achilles tendinopathy can be classified as midsubstance (2-6cm proximal to the insertion) or insertional (within 2cm of the insertion) with the main difference being the location of pain. Injury to the tendon occurs along a continuum, with changes to the tendon structure. Midsubstance injuries are the most common among both active and inactive people. Typical presentation includes a gradual onset of pain that is often worse in the morning and improves with 5-10 minutes of activity.
Causes
Multiple intrinsic and extrinsic factors can influence the tendon’s response to the subjected load. Therefore, the tendon’s capacity for load is specific for each individual and their activities. The primary mechanism for tendinopathy is overload of the tendon, with compressive overload proposed to cause the tendinopathic process within the tissue. Essentially a failed healing response is evident, with an increase in the noncollagenous matrix, leading to increased susceptibility to damage (Maffulli et al. 2020). Typically, this condition causes pain, swelling and stiffness in the Achilles tendon.
Risk Factors:
- Increased BMI, adiposity, high cholesterol, diabetes mellitus
- Previous tendinopathy and genetic predisposition
- Increased distance, speed, and frequency of training
- Recent change in footwear or training surface
- Weakness and poor endurance of ankle plantar flexors & knee flexors
- Altered biomechanics/muscle activation along the kinetic chain.
Treatment and evidence:
Physiotherapy will help in the management of tendon loading. Treatment will include soft tissue work to help reduce muscle overactivity and will providing education regarding load management and activity modification and will also include exercise prescription.
Exercise is vital for effective treatment in order to progressively load the muscle tendon unit. The ideal exercise program will allow the tendon to develop tolerance to load, as opposed to an actual change in the tendon structure. An initial reduction in aggravating loads will be advised to ease symptoms, followed by a progressive increase in load, to improve tendon capacity. For an irritable tendon, isometric exercises can help to reduce pain, whilst allowing a load stimulus.
As progression is made, slow heavy strengthening, eccentric loading, and sport specific loading if applicable should be included. Our physio’s will also assess the kinetic chain and muscle activation patterns. Weakness along the kinetic chain will often lead to tendon overload and thus Achilles tendinopathy so it is vital that it is assessed and treated as needed. To achieve the best outcome exercise needs to be targeted to the individual, the stage of pathology and patient’s functional demands and goals (Malliaras et al. 2013).Other adjuncts to exercise and manual therapy that may be used include ice, taping, heel raises and footwear modifications to assist with symptom control. Ultimately though, the tendon must be loaded and complete rest is discouraged (Brukner and Khan, 2017, Cook and Purdam et al. 2012).
Exercises to help Achilles tendinopathy
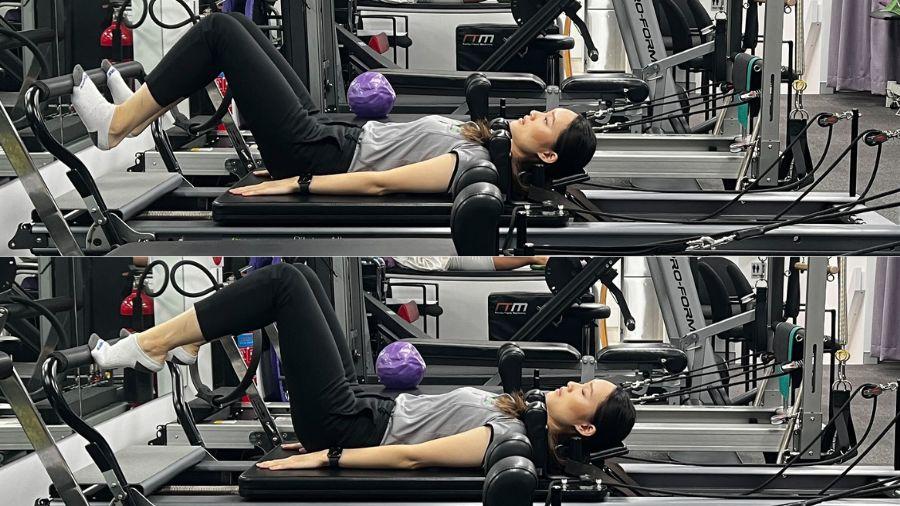
Soleus raises on Reformer
Aim: To strengthen up the Soleus muscle
If the soleus muscles are not strong enough to handle daily activities, the achilles is often overloaded instead causing irritation. Strengthening the soleus muscles, similar to the calf muscles improve push off when walking and running, and provide shock absorption for the lower limb.
How do I do the exercise: Lye on your back on the reformer, place both toes on the foot bar. Push through your feet to slide the reformer, slightly extending your legs. Keeping the knees bent in a half squat position, drop your heels below the bar and push to raise the heels up. The level of difficulty and intensity can be varied by adjusting spring resistance or by progressing to one legged raises.
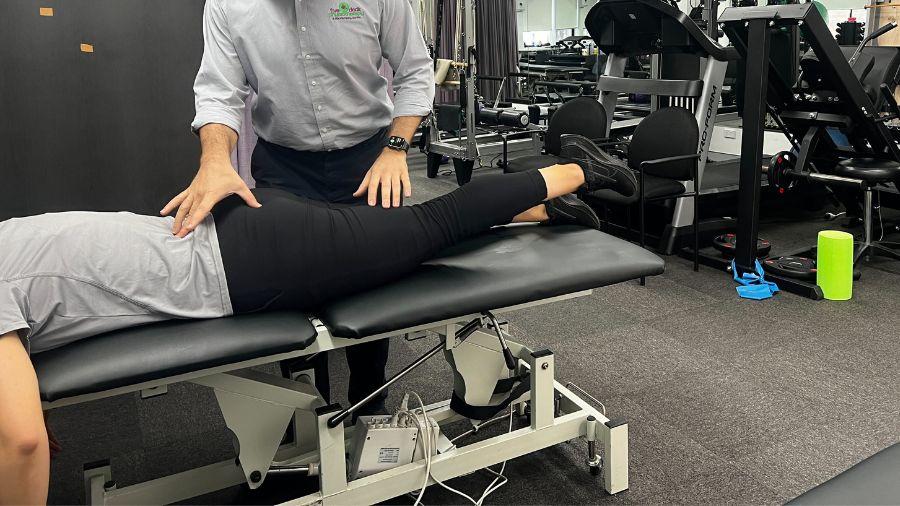
Prone hip extension
Aim: Improve posterior chain strength (Gluteus maximus, hamstring and back extensor strength) & core stability.
During walking, pushing off the back leg to step forward involves posterior chain strength. If these muscles are not strong enough, the Achilles takes more load than usual, and can lead to a tendinopathy. Improving the strength of these muscles will assist with push off.
How do I do the exercise: Lying on your tummy engage your core muscles, actively squeeze your glute muscles and lift your leg off the bed. The aim is to instigate the movement with your gluteal muscles and not your hamstring or back muscles. This activation sequence is very important so that extra stress is taken off other parts of the kinetic chain.
Foam Roller Calf muscles
Aim: to reduce muscle tightness and overactivity in the calf muscles.
With an Achilles tendinopathy the calf muscles often become overactive and tight, however when you stretch these muscles out you can place compressive forces on the tendon eliciting pain, thus by using the foam roller we can reduce tightness without compressing the tendon.
How do I do the exercise: Sit with your leg stretched out. Place the foam roller under your calf muscle. Take the weight through your hands and roll your lower leg back and forth over the roller, massaging the area to reduce tightness and overactivity, thus taking stress off the Achilles tendon.


