Have you ever experienced lower back pain?
Chances are that you have, as lower back pain (LBP) is the most common musculoskeletal injury with reports that 80% of the population (Holmes et al, 2015) will experience LBP at some point in their life and every year up to 36% of the population will have an episode of LBP (Hoy et al, 2010).
Unfortunately, if not identified and treated early, up to 20-30% of episodes of lower back pain can become persistent and chronic, impacting on physical function and quality of life. However, this doesn’t have to be the case as Physiotherapy is shown to be effective in improving symptoms, function, and quality of life for both acute and chronic back pain cases. This is achieved through education, progressive exercise, manual therapy, and Cognitive Behavioral Therapy (CBT).
What causes lower back pain?
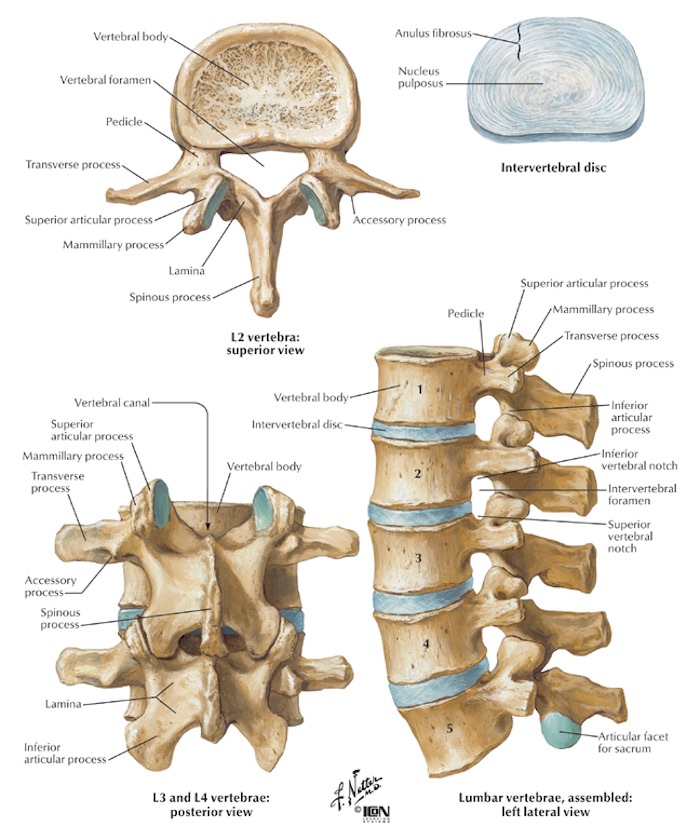
90% of LBP is classified as “Non-Specific” LBP (Koes et al, 2006) and attributed to a musculoskeletal injury to the joints, muscles and/or soft tissue structures. It may be a result of an acute injury (fall, lifting, twisting), poor posture, a change in load or due to repetitive stressful movements. Most commonly there is poor muscle activation & strength, joint stiffness and/or altered biomechanics impacting on back function. Only 2% of cases are associated with more serious “red flag“ pathologies.
Risk factors of lower back pain
- Sedentary behaviours—long periods of sitting (office population) or lying down (long hospital stay), obesity, sleep disruption, smoking, alcohol
- Sudden increases in physical activity and load
- Increased psychosocial stress & anxiety
- High volumes of sustained and repetitive loading of the spine & musculature (labour intensive jobs—builders, tradies, truck drivers, landscapers etc.)
- Poor lifting techniques, altered biomechanics and poor muscle recruitment patterns
Signs and symptoms
Depending on the underlying cause of the pain, the symptoms can present differently. Some common symptoms include:
- Pain that is dull or achy, usually localized to the lumbar spine
- Stinging, burning pain that radiates from the low back to the gluteals and legs. It can also refer to the lower legs or feet; and can include numbness or pins and needles
- Restricted lower back movement associated with pain
- Muscle spasm, overactivity or tightness in the low back and hip muscles
- Pain that worsens with prolonged postures i.e. sitting or standing
- Disc related pain is often present with flexion movements such as bending, sitting and lifting.
- Facet joint related pain is often associated with extension and rotation movements like standing up straight, walking, leaning backwards or going from sitting to standing
- It is not uncommon that disc and joint related issues occur together

Examination and diagnosis
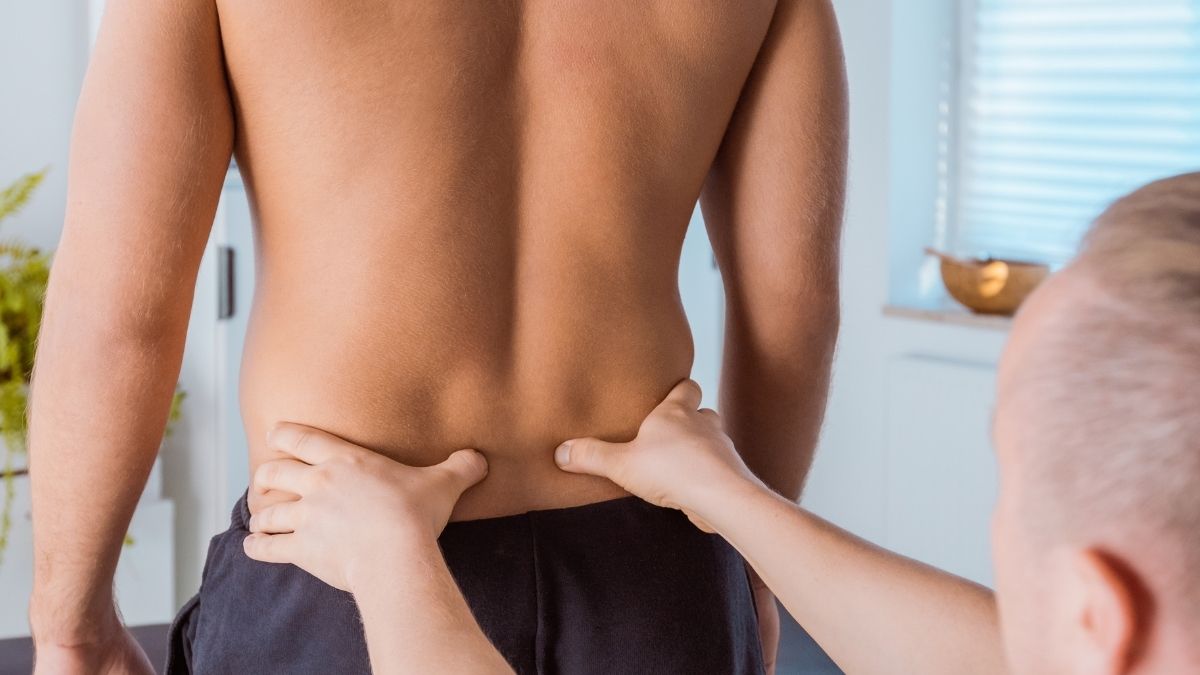
Our physiotherapists will conduct a thorough assessment to determine the involved structures and provide treatment accordingly. Our assessments take into consideration the onset of symptoms and whether they came on slowly, or were a result of trauma, posture, a spike in load or an incorrect lifting technique.
We will also investigate the underlying muscle activation patterns, so the biomechanical causes of low back pain. For instance, we look at hip and pelvic stability during static and dynamic tasks as well as strength of the gluteal and core muscles as these factors impact on the ability of the lumbar spine to handle loading through activities like bending and lifting. Poor stability and control can have a significant impact on recurring episodes of acute back pain, and therefore these structures will be assessed thoroughly (as will the whole kinetic chain). A postural assessment is also performed to analyse its impacts on the back.
During our assessment our physiotherapists will also help you to determine functional goals or activities that you want to get back to doing where appropriate. This ensures that we tailor our treatment to each person, helping guide our patients to a safe return to their ADL’s, sport, hobbies and work situations. Our aim is to also help minimise recurrent back issues and reduce secondary injuries that result from compensatory movement patterns.
Our physiotherapy assessment will not only aim to correctly classify and diagnose LBP, but also rule out any red flags or neurological conditions that require immediate referral. Following a comprehensive assessment our physios are able to get an understanding of the underlying biomechanics and the compensation strategies that are contributing to each individuals symptoms.
Where needed, investigations like X-Ray, CT and MRI can assist with this, and we will regularly liaise with the patients GP where necessary. Bear in mind that a study by Brinjikji et al. 2015 demonstrated degenerative spinal changes were present on imaging in asymptomatic patients (people without back pain) in all age brackets above 20 years, indicating that imaging is not always required. Current global guidelines only recommend imaging in cases where serious pathology or radiculopathy (neurological symptoms) is suspected, or if no improvement is seen after 4 weeks of physiotherapy treatment (Kamper et al, 2018).
Physiotherapy Management
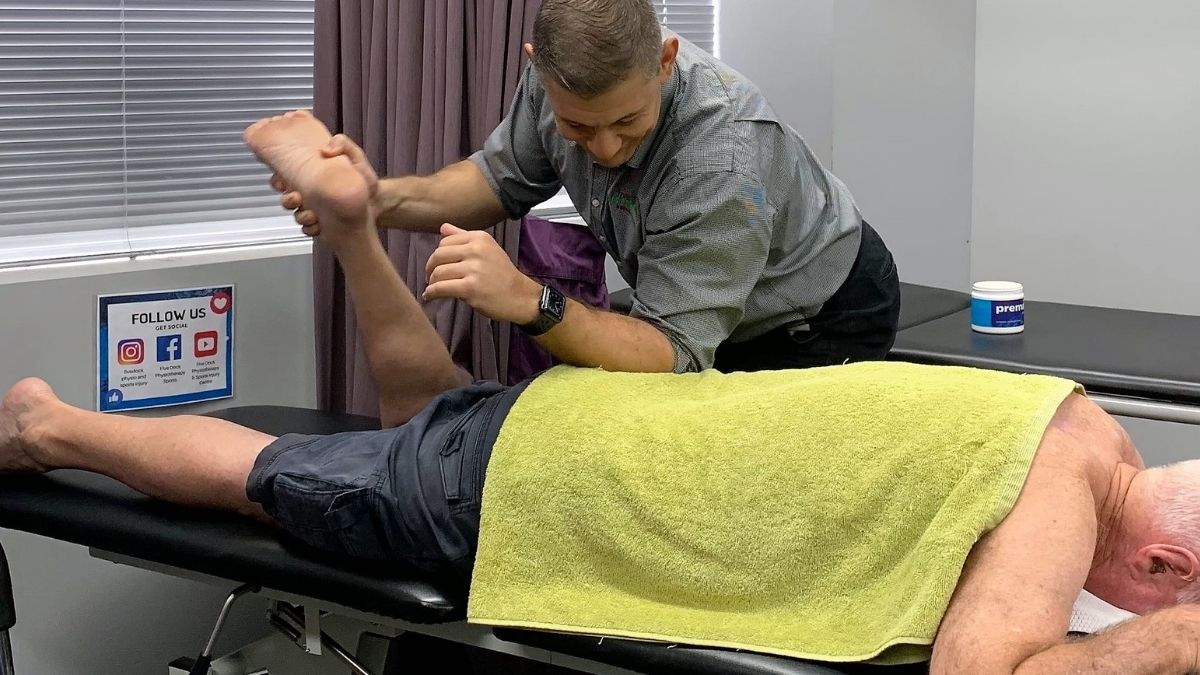
Physiotherapy is important as a first line intervention for LBP. Physio treatment of LBP often involves a combination of manual therapy, a progressive exercise program, CBT, education and advice. Manual therapy is particularly useful in the acute stage of recovery and can help to reduce symptoms by decreasing muscle overactivity and improving joint mobility. Education regarding appropriate movements, posture, ergonomics, load management and the Do’s and Don’ts for the patient’s specific back issue is essential to accelerate recovery.
Exercise plays an incredibly important role. In the early stages of rehabilitation certain exercises aim to get our patients moving again and provide relief, whilst other exercises help restore muscle activation patterns including core control. As progress is made, our physiotherapists will start to focus on strength, and progress motor control and endurance exercises. This progression through rehabilitation is essential to getting patients back to achieving their goals whether it be work/sport/life and preventing recurrences and all of our exercises prescribed have the patients goals in mind. Depending on the patient’s goals we will often guide this process and empower independence by taking our patients into the gym or leading them through Clinical Pilates based exercises often using the Cadillac Reformers we have in clinic. All patients are discharged with a home exercise program to help minimize recurrent episodes of lower back pain.
Evidence
Research into lower back pain has consistently shown that conservative management, incorporating the key elements of education, advice, activity modification, manual therapy and a guided progressive exercise program to be the best practice treatment as evident by the overview of the current guidelines by Oliveira et al, 2018 and Owen & Miller et al, 2020. A variety of exercise programs have been shown effective with Wang et al, 2012 and Shamsi et al. 2015 demonstrating improvements in both pain and disability with either core specific or general low back exercise programs. Brukner et al, 2018 supports the use of manual therapy in relieving symptoms, improving segmental mobility and relaxing muscle spasm. Gladwell (2006) supports the use of Pilates to improve general health, pain levels, sports specific function, flexibility, and proprioception in individuals with chronic low back pain whilst Gorden et al, 2016 concluded a multi factorial approach of strength, flexibility, stability and aerobic fitness to be most beneficial.
A systematic review done by Lin et al, 2016 studied the effects of Pilates in non-specific chronic low back pain patients, they concluded that Pilates has a significant improvement in pain relief and functional capacity, comparable to other lumbopelvic stabilization exercises. The authors also proposed that to achieve a clinical analgesic effect and enhance functional capacity, patients with chronic low back pain need to adhere to a Pilates exercise program with the frequency greater than 2-3 times a week, with each session lasting at least an hour, for a minimum cumulative training of 20 hours.

Conclusion
Although LBP can affect such a high percentage of the population, it is reassuring to know that both chronic and acute bouts of LBP can be significantly improved with holistic physiotherapy treatment, and this is supported by the research and evidence. Unfortunately, though, there is no cookie cutter approach to exercises or treatment. Prescribing the right exercises based on the assessment, progressing them accordingly and giving the right advice to the patient takes careful consideration as not all back pain is alike, and the wrong advice or exercise prescription can unfortunately irritate a patient’s symptoms. Similarly, exercises will often vary based on the goals that a patient has.
Our physio’s however use careful clinical reasoning guided by our ongoing reassessment of the patient to determine appropriate exercise prescription and progression, aiming to not only help our patients get out of pain and achieve their goals, but we also aim to help our patients prevent a relapse of symptoms.
The last bit of advice is that if you or a loved one is experiencing lower back pain, don’t delay getting it looked at. The sooner our physios are able to examine your back, the quicker we can help you get relief and guide your recovery so that you can back to all the things that you love or need to do.
………
ARE YOU OR A LOVED ONE TROUBLED BY BACK PAIN?
GET A COMPREHENSIVE ASSESSMENT & TREATMENT WITH OUR TEAM OF AMAZING PHYSIO’S.
- Get crystal clear about what’s causing your Back Pain.
- Find out the most important steps for you to get pain free fast!
- Understand how to manage your normal activities without suffering the consequences of pain
- Find out the simple yet essential exercises that can help you get lasting and fast relief
- Leave the session with the confidence of knowing exactly what to do to get symptom free and back to living life without pain
Please contact us on:

