Anatomy
The calf muscles comprise of the gastrocnemius and soleus muscles. The gastrocnemius is one of the main plantar flexors of the ankle. It is comprised of two muscle bellies, with the medial head having a mechanical advantage. It is therefore able to generate more force, making it more susceptible to injury compared to the lateral head. “Two-thirds of calf injuries occur at the junction of the fascia between the medial head of the gastrocnemius and the soleus. Injuries to the lateral head of the gastrocnemius occur in up to 14% of patients in some case series, but injury may occur anywhere from the proximal origin to the mid-belly to the fascial junction with the soleus.” (Bright et al 2017)
Causes of a calf tear
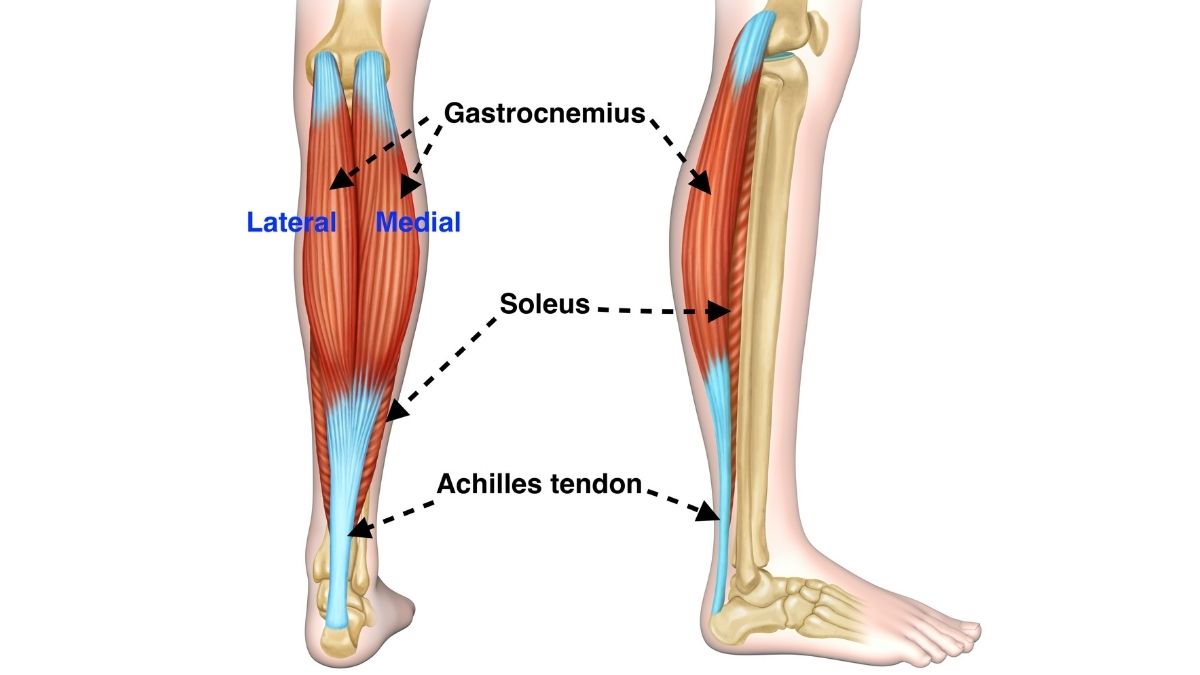
The gastrocnemius muscle assists with explosive movements, and therefore injuries generally occur after a sudden movement such as accelerating in a run or jumping. The Soleus muscle lies beneath the gastrocnemius and has more of a role in endurance activities such as long distance running and prolonged walking. The Soleus muscle is therefore more prone to overtraining injuries and the tears occur over longer periods rather than a sudden movement.
How are symptoms described?
Similar to the history of an Achilles tendon rupture, people often think they’ve just been hit in the leg by a ball or other object and potentially hear a “pop” or “snap”. In nearly all cases, they will feel a sudden pain in the back of their calf particularly at the musculotendinous junction. If the Soleus muscle is damaged pain might be felt lower in the leg and when contracting the muscle against resistance with the knee bent.
Diagnosis & Examination
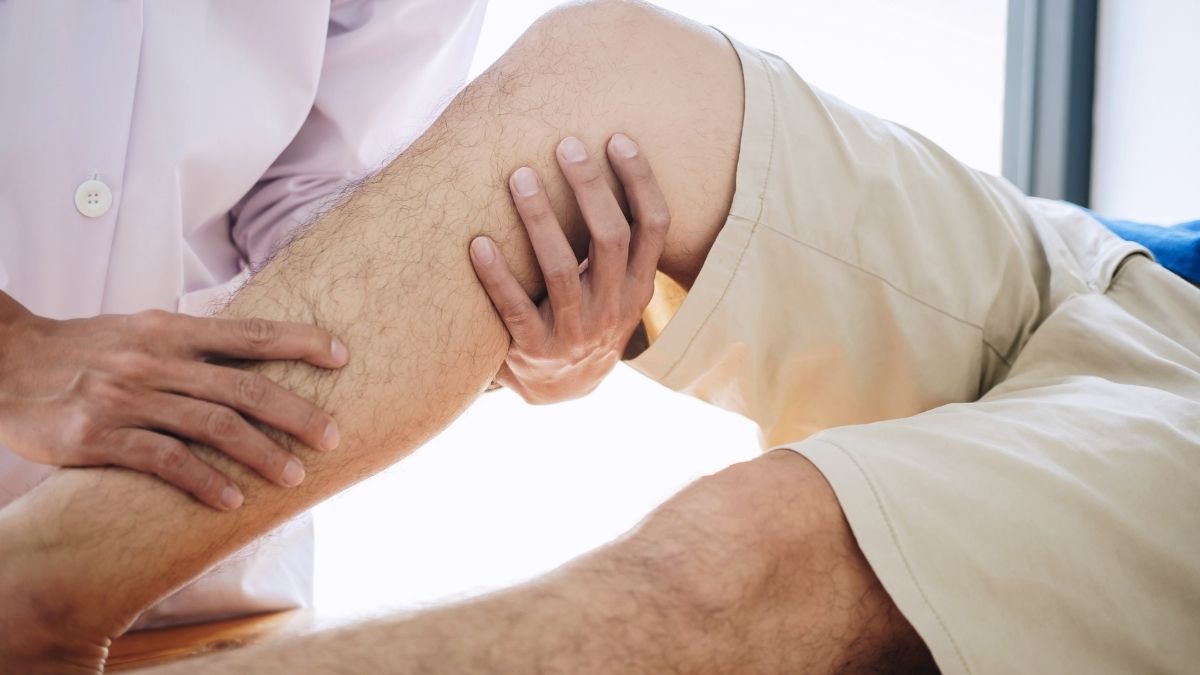
Physiotherapists are highly qualified professionals with expert knowledge and skills in the diagnosis of muscle injuries. A thorough subjective and objective examination performed by a Physiotherapist is sufficient to diagnose a torn calf. Early diagnosis is key to ensuring that initial management is tailored to the specific structure that is injured.
A thorough examination will reveal the following signs: usually a patient will walk into the clinic with a antalgic gait, depending on the severity of the tear, they may be unable to weight bear on the injured leg at all. In higher grade tears there may be a palpable gap over the site of the tear and depending on how acutely they present there may be associated bruising and discolouration of the skin. The patient will also lose range of motion in dorsiflexion and plantarflexion. Typically, they will be unable to raise on their toes performing a double or single leg calf raise however this also depends on the grade of the tear. “The vast majority of calf injuries can be diagnosed and managed without any additional imaging” (Bright et al 2017). Occasionally an ultrasound can be used to determine the size of the tear however they are not always accurate, and although clinically a tear has been diagnosed sonographers can miss these from time to time. Further imaging such as MRIs are rarely utilised unless differential diagnoses are suspected.
Differential Diagnosis
Carrying out a thorough objective examination is important to exclude other pathologies that can occur in the same region.
Examples include:
Deep vein thrombosis – a very serious pathology that can result in a fatal pulmonary embolism—can occur with severe calf tears.
- Plantaris tear – a small muscle which is actually absent in 8-12% of the population. Although not vital for function, it can be very painful when torn or ruptured resulting in limping and altered biomechanics
- Achilles rupture – a very serious pathology requiring immediate orthopaedic review
- Compartment syndrome – painful condition with increased pressure within muscles and fascia, compressing muscles, nerves and vascular structures.
Treatment and Evidence
Initial stages of treatment aim to reduce pain, swelling and further injury. Crutches may be necessary for patients that are unable to weight bear. They should only be used for a short amount of time as early mobilisation allows muscle fibres to regenerate and organise more effectively and prevent DVTs forming (Hsu & Chang, 2021). Within 10 days, scar tissue that has formed over the tear will have the same tensile strength as normal muscle and gradual loading can begin (Dixon et al 2009). Ice is useful in the acute stage and patients will often benefit from the use of Tubigrip compression to support the injury.
In the early stages as symptoms improve it is important to restore normal walking patterns to avoid developing compensations. Our physiotherapists will help our patients activate and use the correct muscles with exercises and gait retraining. Incorporating an exercise program targeting range of motion, strength, endurance and motor control/balance is essential for recovery and should be implemented once symptoms allow (Hsu & Chang, 2021). Strengthening exercises will be provided for the muscles in the calf, quads and glutes to address biomechanical compensations from the antalgic gait. Exercises are progressed in difficulty until the injured leg’s strength, endurance and power is comparable to the non-injured leg. Time to return to activity and re-injury rates were found to be markedly reduced in those patients who completed physiotherapy rehabilitation compared to rest alone (Jones, S et al. 2019)
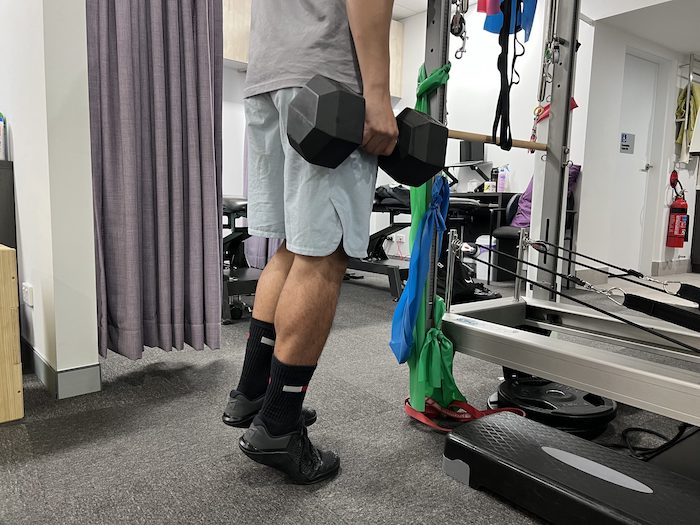
In the clinic, we see patients regain their ability to walk normally for day to day activities but do not have the adequate power to perform a quick sprint or jump. Power is often overlooked and if not trained adequately, a larger re-tear occurs when trying to perform these activities. Plyometric exercises as well as a graded sprinting program is a vital part of physiotherapy rehabilitation to ensure safe return to sport. Our physiotherapists will target rehabilitation to meet patient specific goals ensuring good long-term outcomes and prevention of secondary kinetic chain injuries.

Do you have a calf tear inury?
GET AN ASSESSMENT & TREATMENT WITH OUR AMAZING TEAM OF PHYSIO’S.
- Get crystal clear about what’s causing your injury or pain
- Understand what activities you can do without suffering consequences of shoulder pain or instability
- Find out the simple yet essential exercises that can help you achieve amazing result
- Leave the session with the confidence of knowing exactly what to do to get symptom free and back to living life to the full