Cervicogenic headaches are a common musculoskeletal problem linked with neck pain and neck dysfunction. The Headache Research Foundation (2020) revealed that 90% of intermittent headaches and migraines can be attributed to neck pain. These are known as cervicogenic headaches.
Cervicogenic headaches are a type of secondary headache that derive from the neck. Symptoms arise from the dysfunction of joints, muscles and nerves surrounding the upper cervical spine (neck).
Prevalence
Cervicogenic headaches are commonly present in individuals that adopt poor posture for prolonged periods. According to Seffah et al., 2023, combining an inadequate ergonomic workstation set-up, excessive use of technology and sedentary lifestyle can significantly attribute to the increasing prevalence of neck pain and cervicogenic headaches presenting to doctors and physiotherapists alike.
Cervicogenic headaches may also occur secondary to degenerative changes in the cervical spine such as osteoarthritis or degenerative disc disease (Oakley et al., 2019). The onset of these headaches can also be as a result of trauma such as a fall or whiplash. Current research underpins this strong association with 54%-66% of individuals who suffer whiplash injuries also experiencing headaches (Costa De Almeida et al., 2023)
Common Signs & Symptoms
- Headache associated with neck pain and stiffness
- Neck tightness/active trigger points
- Pervious history of having sustained trauma to the neck (fall, whiplash or concussion)
- Pain on one side of the head
- Pain that often radiates from the back to the front of the head or pain that can radiate into your eyes
- Potential of vague arm/shoulder pain on the same side
- Onset of headache following prolonged postures, positions or repetitive movements.
Diagnosis
Cervicogenic headaches can be diagnosed by our physiotherapy team through a combination of subjective history and objective examination in the initial consultation. Our evaluation will rule out other possible types of headaches or pathologies that could be affecting one’s musculoskeletal structure.
Common objective findings when assessing for cervicogenic headache often include:
- Pain with moving the neck (although sometimes patients present with full movement)
- Pain with prolonged postures
- Active trigger points in the cervical muscles that can directly refer headache symptoms as a result of muscle tightness/tension
- Extended upper cervical spine (forward neck posture), with associated postural muscle weakness.
- At times a dowager’s hump may be preset or alternately an increased thoracic kyphosis with protracted scapulae
- Muscle imbalance noted and scapula-humeral dysfunction often present
- Reduced endurance of the deep neck flexor muscles
- Palpable joint dysfunction and symptom reproduction on joint palpation of the upper cervical or neck segments (Occiput – C3).
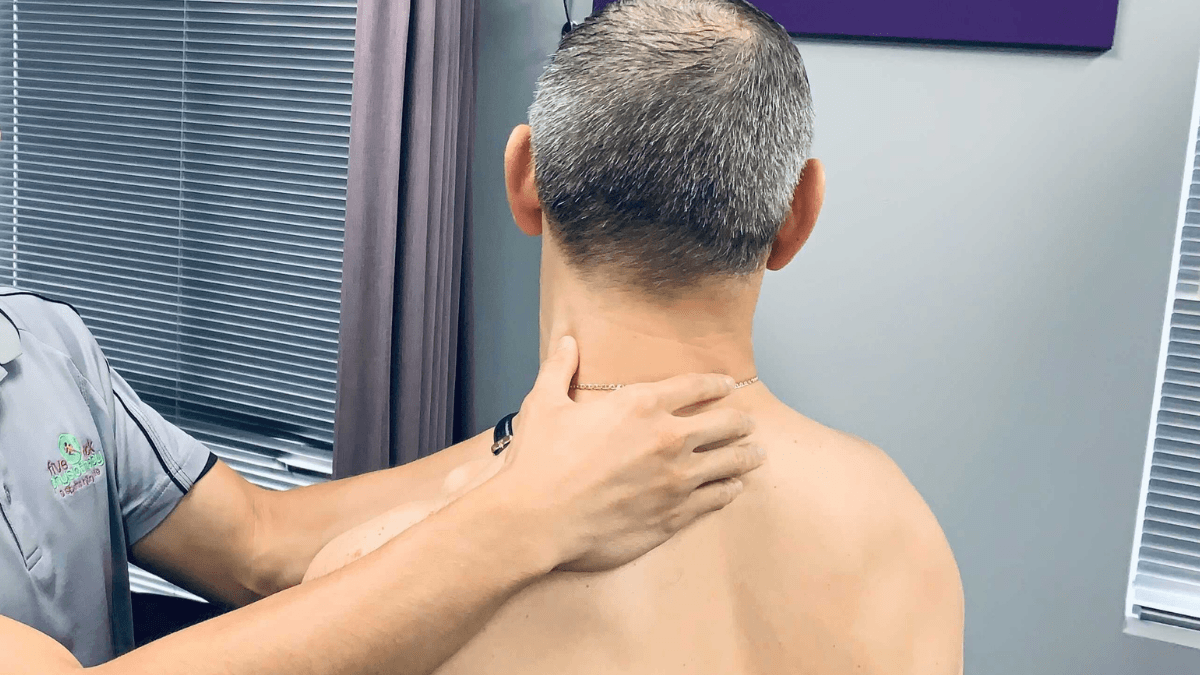
Treatment
There is strong correlation between physiotherapy intervention and management in effectively treating cervicogenic headaches (Al Khalili et al., 2022). Therapy for cervicogenic headaches involves a comprehensive treatment plan which aims to promote movement, improve posture, and strengthen the neck and shoulder muscles. Research indicates the beneficial nature of manual therapy (soft tissue work and joint mobilisation) in the initial stages of treatment (Jin et al., 2021). This assists in releasing overworked muscles as well as enhancing mobility of stiff/hypomobile joints. However, it is important that manual therapy and exercise therapy are completed simultaneously to receive the best treatment for cervicogenic headaches (Demont et al., 2022).
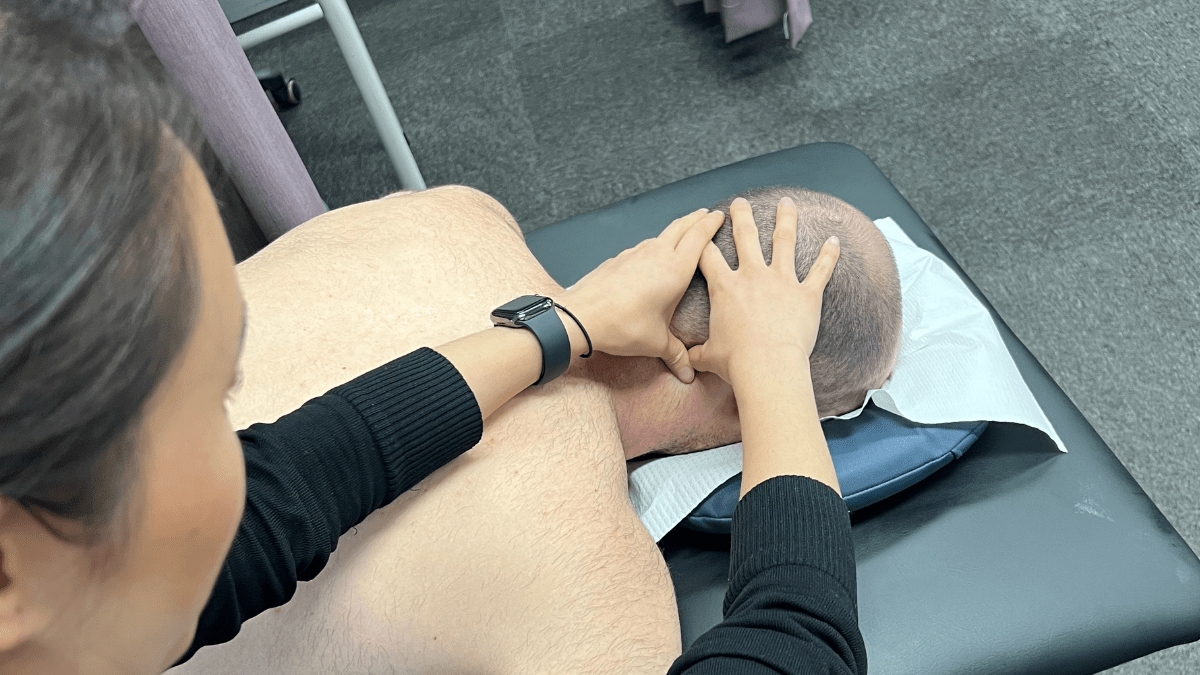
Manual therapy techniques utilised include joint mobilisation for the cervical segments, soft tissue massage and trigger point releases to the superficial and overactive neck muscles. Sustained mobilisation of the affected joints and release of the tight neck muscles have been shown to resolve cervicogenic headaches and improve neck movement. Releasing these muscles that frequently have active trigger points when palpated can also assist in alleviating a patient’s headache symptoms.
In addition to manual therapy, a comprehensive individualised exercise program will be prescribed to specifically target the individual’s impairments to address the primary cause of cervical dysfunction. Rani et al., (2022) reported that “spinal mobilization and postural correction exercises are effective in the management of cervicogenic headache”. Exercises embody a combination of deep neck flexor strengthening, shoulder/scapular retraining, postural endurance exercises and core strengthening. Ultimately, the program aims to correct an individual’s biomechanics which may be predisposing them to a cervicogenic headache. Studies reveal the benefits of pilates exercises in treating cervicogenic headaches through significant increases in range of motion, postural training as well as decreases in neck and shoulder pain (Phupanich et al., 2020) and Lee et al., (2016) report that “headache patients with neck and shoulder pain can decrease their pain and increase cervical ROM by practicing Pilates exercises”. Stretching exercises are another vital part of the exercise program, as they can provide relief for overactive muscles and improve muscle flexibility. Advice from the treating physiotherapist regarding workstation set up, technology use and posture in general is also a critical aspect of treatment.
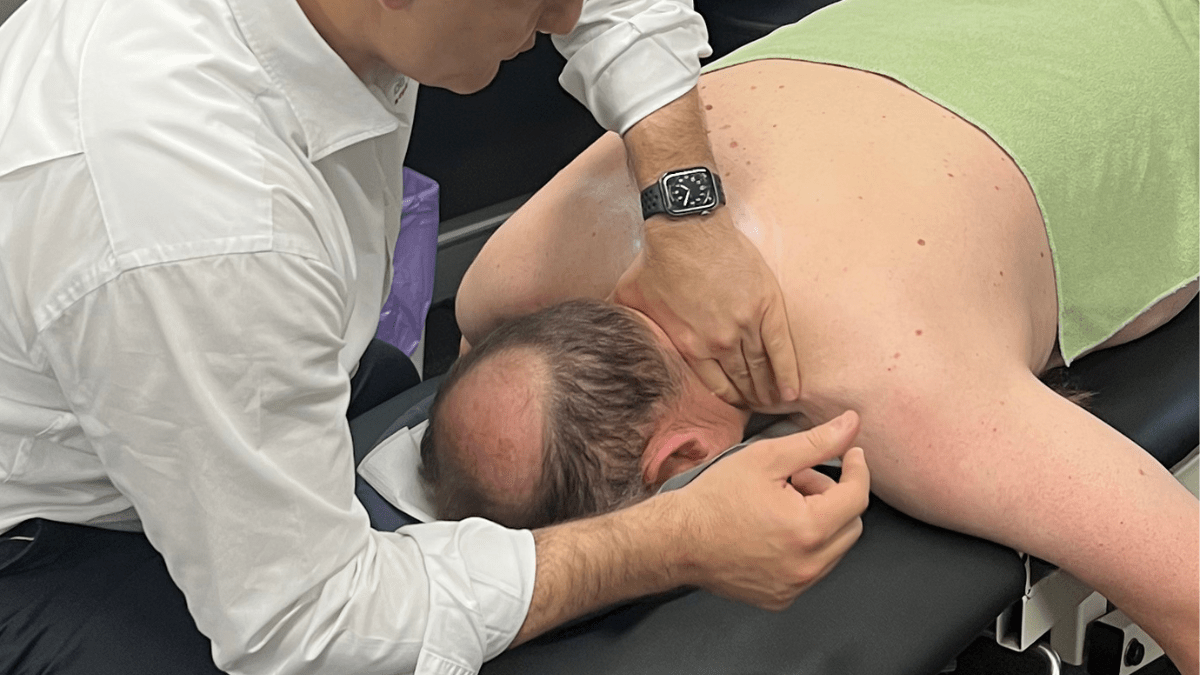
Things Physio’s use to improve Cervicogenic headaches.
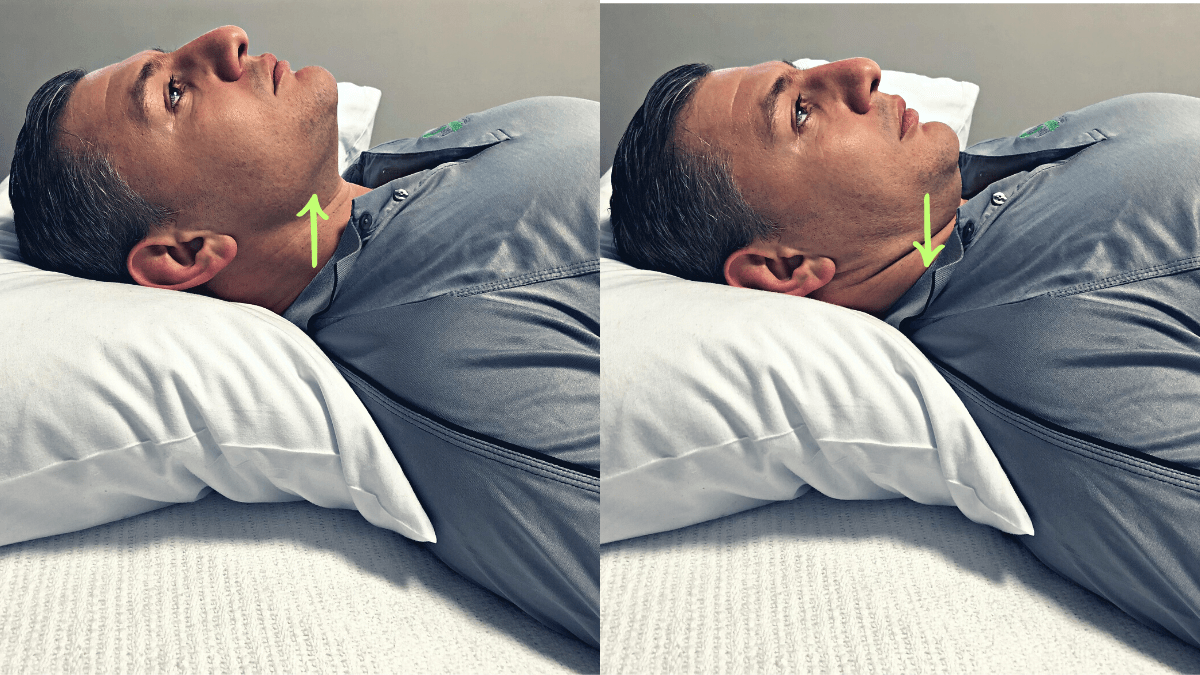
Deep Neck Flexor training:
Improve activation, endurance, and contraction of the deep cervical flexors. Simply lye on your back with head on a flat pillow or folded towel so the head is in a neutral position. Gently and slowly nod the head as if saying “yes”, but only moving a small amount. Hold 5 seconds for 10 reps. It should feel very subtle and the big muscles in your neck should not contract. Increase difficulty by increasing hold time.
Trigger ball self-release:
A trigger ball can be used as self-treatment tool to help release overactive muscles that can refer cervicogenic headaches. Simply place the ball over the point of tension to get relief or add in an active release by simply turning your head.

Horizontal extension on the reformer:
In high kneeling on the reformer engage your core muscles. Place your hands in the straps starting at your midline and then pull the straps and your arms apart training your upper back muscles and improving your posture. Adjust springs to change level of difficulty.