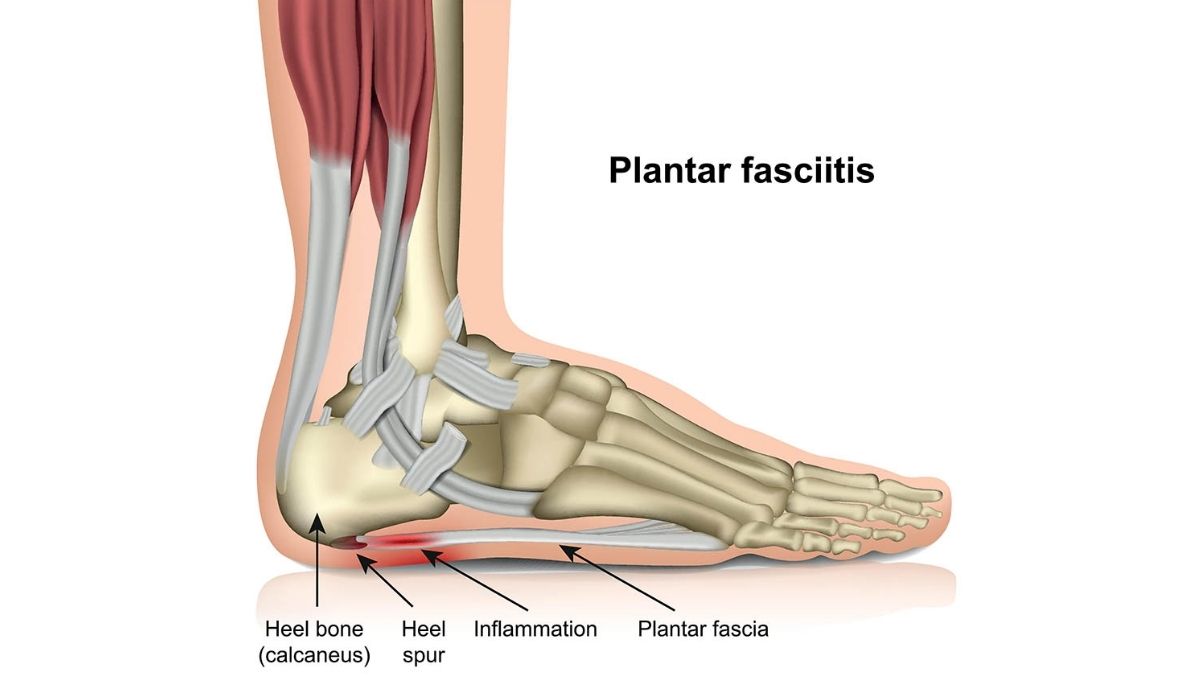
Plantar fasciopathy (often referred to as plantar fasciitis) refers to localised pain at the plantar fascia’s insertion into the calcaneus (heel bone). It involves inflammation of this thick band of tissue often due to overload of the plantar fascia.
Common tests for diagnosis
Below are five tests we use in the clinic to commonly diagnose plantar fasciaopathy:
1. Palpation: Tenderness over the origin of the plantar fascia (tubercle of the calcaneus) , medial ankle and fat pad. This can be located to the inside and bottom of the heel.
2. Functional plantar flexion: Pain in the region of the plantar fascia with a single leg calf raise (raising up on toes on one leg).
3. Restricted range of motion through the ankle, and restricted big toe extension can lead to increased tension through the plantar fascia
4. Windlass test: A positive Windlass test occurs after reproducing arch/heel pain through passive great toe extension (therapist moving big toe towards head)
5. Poor Biomechanics:
- Poor single leg stability or a valgus buckle on a single leg squat indicating poor gluteus medius control
- Poor posterior chain firing patterns affecting push off during walking/running gait
- Calf weakness affecting push off and shock absorption
- Overpronation of the foot leading to increased pressure in the tibialis posterior and intrinsic muscles of the foot

Treatment
Physiotherapy rehabilitation is critical for effective management of plantar fasciopathy. Our treatment targets strategies for effective pain relief, includes stretches and strengthening exercises, provides education and activity modification and we employ strategies to help prevent recurrences of this condition.
Footwear: Adequate arch support is required to reduced the overstretching of the plantar fascia during gait. Appropriate running shoes, orthotics or a moonboot may be utilised to assist arch support.
Load management: Adjusting the patient’s time on feet with activity to reduce pressure on the plantar fascia, allowing timely healing
Taping: Supportive tape can act to support the arch and reduce over-stretching of the fascia during gait
Soft tissue therapy: Massage of the plantar fascia and local muscles will reduce stiffness of movement and provide pain relief to the area. Self release strategies with a spikey ball bottle can also help.
Exercise: This consists of strength training by improving endurance of the intrinsic foot muscles, tibialis posterior and calf muscles. This then leads to an exercise program addressing biomechanical issues in the lower body such as gluteal and core dysfunction. The rehab program will be progressed according to level of function required for the patient to achieve their goals, whether it be sporting ambitions or functional tasks such as walking for work or walking the dog.

Can the Pilates Reformer be used to rehabilitate Plantar Fasciopathy?
Although we wouldn’t typically only use Pilates exercises to rehabilitate plantar fasicopathy, when use as an adjunct to physiotherapy or when patients are already undertaking Clinical Pilates whilst struggling with plantar fasciopathy, there are several exercises we can do on the Pilates reformer to strengthen the affected muscles and reduce load through the plantar fascia. This can improving strength and endurance of the lower limb, thus improving load tolerance. These are some exercises that may assist with the recovery of Plantar Fascia issues:
Calf Raises
Aim: To strengthen up the calf muscles
If the calf muscles are not strong enough to handle daily activities, the planta fascia is often overloaded, instead causing irritation. Strengthening the calf muscles improve push off when walking and running, and provide shock absorption for the lower limb, thus taking stress off the plantar fascia.
How do I do the exercise: Lie on your back on the reformer, place both toes on the foot bar. Push through your feet to slide the reformer and extend your legs. Keeping the leg straight, drop your heels below the bar and push to raise the heels up. The level of difficulty and intensity can be varied by adjusting spring resistance or by progressing to one legged raises.

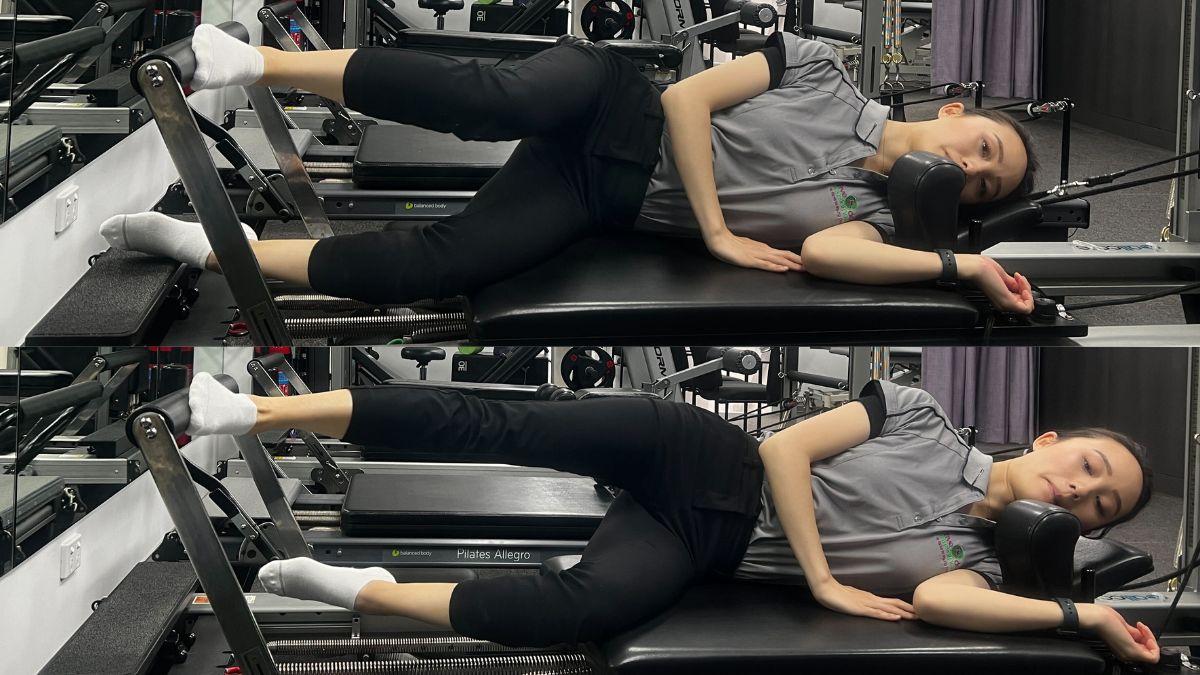
Side-lying Single leg Squat
Aim: Improve Gluteus Medius stability & endurance, helping to prevent a valgus knee buckle which often leads to overpronation, and an increase in stress through the plantar fascia. Also improves quadricep strength, assisting with push off during walking and running.
How do I do the exercise: Lying on your side on the reformer with your hips facing forward, place the top leg on the foot bar parallel to the ground. Press out against the foot bar to extend the top leg and move the carriage up, then flex/bend the knee to bring the carriage back down. Ensure that your knee stays in line with your second toe (or lifts slightly towards the sky) as you squat to further target your gluteus medius. Level of difficulty can be adjusted changing spring resistance.
Bridge off foot bar
Aim: Improve posterior chain strength (Gluteus maximus hamstring and back extensor strength) & core stability.
During walking, pushing off the back leg to step forward involves posterior chain strength. If these muscles are not strong enough, the planta fascia takes more load than usual, and can lead to plantar fasciopathy. Improving the strength of these muscles will assist with push off.
How do I do the exercise: Lying down on the reformer, place both feet hips distance apart on the foot bar. Roll the hips up and flatten back against the carriage to tighten the core muscles. Without moving the reformer, raise your hips off the carriage until they are in line with your knees. Return the body back down to the carriage, without moving the reformer. To make the exercise more difficult use less spring resistance.


