The hip is a ball and socket joint formed between the femur and acetabulum of the pelvis. The acetabulum (the concave portion) has a ring of fibrocartilage, known as the labrum, which acts to deepen the hip joint providing more stability to keep the ball in the socket. The labrum also acts as a shock absorber and aids in lubricating the joint. Unfotunately, it is possible for the labrum itself to tear – which can lead to pain as well as restricted movement. 22-55% of patients with hip or groin pain symptoms are found to have a labral tear (Kwon et al, 2022)
Types of Labral Tears
- Degenerative – often associated with aging or repetitive stress, this type of tear involves gradual wear and tear of the labrum over time.
- Acute – labral tears can also less commonly occur after a traumatic injury or with activities that involve twisting, pivoting, or sudden changes in direction such as sport.
- Insidious – sometimes labral tears can occur spontaneously without a clear mechanism, especially if the individual has any structural abnormalities involving the hip joint itself.
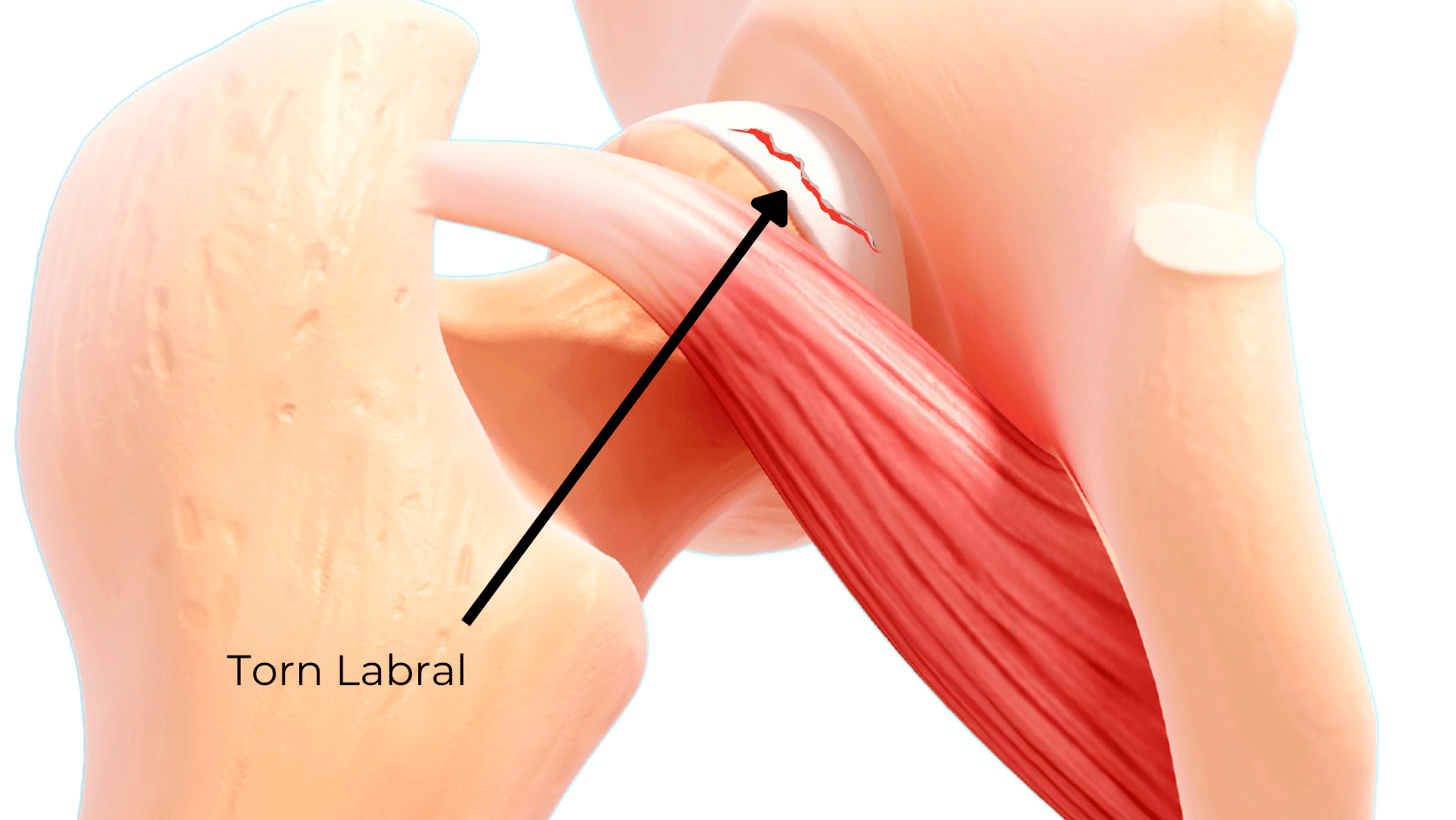
Risk Factors / Causes
- Athletic Activities: Sports that involve repetitive hip movements or sudden twisting motions, such as soccer, hockey, ballet, or martial arts, can increase the risk of a labral tear.
- Structural Abnormalities: Certain structural abnormalities of the hip joint, such as femoroacetabular impingement (FAI), hip dysplasia, or abnormal bone growth (pincer or cam deformities), can predispose individuals to labral tears.
- Trauma or Injury: A direct blow to the hip joint or a sudden forceful movement, such as a fall or a car accident, can cause a labral tear.
- Repetitive Stress: Activities or occupations that involve repetitive stress on the hip joint, such as long-distance running or heavy lifting, may increase the risk of developing a labral tear over time.
- Age and Degeneration: As people age, the cartilage in the hip joint may wear down or degenerate, increasing the risk of a labral tear. Degenerative changes in the hip joint can weaken the labrum and make it more prone to injury.
- Other factors include: Hip joint hypermobility, muscle imbalances, poor biomechanics and genetics.

Diagnosis/Assessment
Physiotherapy assessment plays a critical role in the diagnosis of a hip labral tear. The initial assessment will investigate a subjective history, involving how the injury occurred, as well as current symptoms.
Subjective signs include:
- Pain in the hip or groin, often made worse by long periods
- of standing, sitting or walking or athletic activity
- A locking, clicking or catching sensation in the hip joint
- Stiffness or limited range of motion in the hip joint.
- Functional limitations may include prolonged sitting,walking, climbing stairs, running, and twisting/pivoting
An objective physical examination is then performed. This includes an assessment of the hip range of motion, a screeningof the pelvis and lumbar spine, an assessment of strength and hip stability, and an overall assessment of the kinetic chain. Special tests such as FADIR, FABER, Thomas test and Quadrant test, when positive, can help a physiotherapist’s diagnosis when a labral tear is suspected. An x-ray of the hips and pelvis is often performed to assess for bone changes and an MRI is normally required to confirm a labral tear and assess it’s severity and location.
Treatment for a labral tear may either be in the form of conservative management (non-operative) or surgery (hip labral repair). Research suggests that physiotherapy could be trialled first, however if symptoms continue or there’s a lack of improvement then surgery should be considered. In this instance, the physio would liaise with the surgeon and GP, and if required, develop a pre & post-surgery rehab program.

Treatment
Physiotherapy can greatly help outcomes following the diagnosis of a hip labral tear, regardless of whether being managed conservatively or pre/post-surgery. In the first phase of treatment, it is critical to restore range of motion within the injured hip, whilst also protecting the torn/repaired labrum. Physios utilise a combination of hands-on techniques including soft tissue work and joint mobilisation to improve movement.
Exercises are prescribed to strengthen the deep muscles of the hip that provide stability to the joint, and prescribe exercises to improve muscle activation, and correct compensatory movement patterns. This all serves to help stabilise the hip joint, restore function and support the healing of the labrum.
As the patient progresses, emphasis shifts from general activation of surrounding muscles to further local and global strengthening. Functional exercises and goal-oriented activities are incorporated to enhance balance, proprioception, and overall joint control. Additionally, core stabilisation exercises are crucial to improve pelvic and trunk stability and reduce strain on the hip joint during daily activities.
If surgery is planned, physiotherapy is still very important, as improving strength and function pre-operatively can help to reduce timeframes to achieving goals post-operatively.
Before returning to sporting activities, plyometric and sports-specific drills will also be undertaken to ensure the labrum and hip in general can tolerate higher demands. In our clinic, strength testing is also performed using the AxIT Force plates and Dynamometers to ensure adequate strength, and good force and power production.

Evidence
A systematic review by Reiman et al. (2014) suggests that conservative management can lead to significant improvements in pain and function for patients with hip labral tears. Exercise therapy, in particular, is highlighted as a key component of successful management. A study by Lewis et al. (2018) demonstrated that a structured physiotherapy program focusing on muscle strengthening and movement retraining significantly improved patient outcomes compared to usual care.
Research indicates that while conservative treatment can provide symptom relief and functional improvement, some patients may still require surgical intervention if conservative measures fail. Hyland et al (2023) conclude that “comprehensive non-operative management should be pursued prior to consideration of surgical intervention.” Performing a thorough examination and obtaining a diagnosis early is vital to directing patients towards the best possible management and outcome.
Exercise
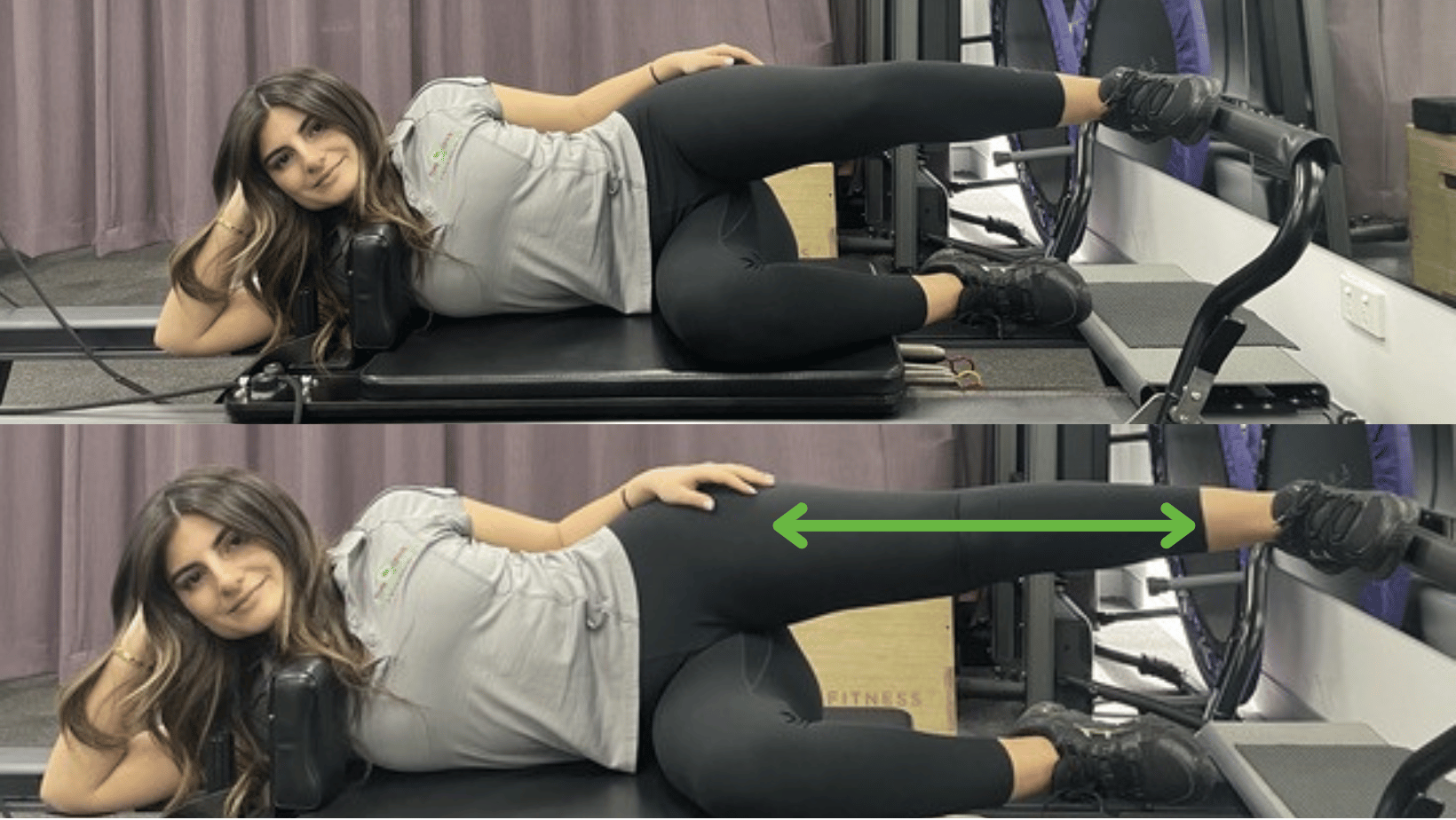
Single leg squat on Reformer
Aim: Improve gluteus Medius and core strength
How: Lay on one side with the top leg on the foot bar. With your core engaged push the carriage away and return slowly to the starting position. Ensure that your knee tracks in line with the second toe. Increase resistance by adjusting springs
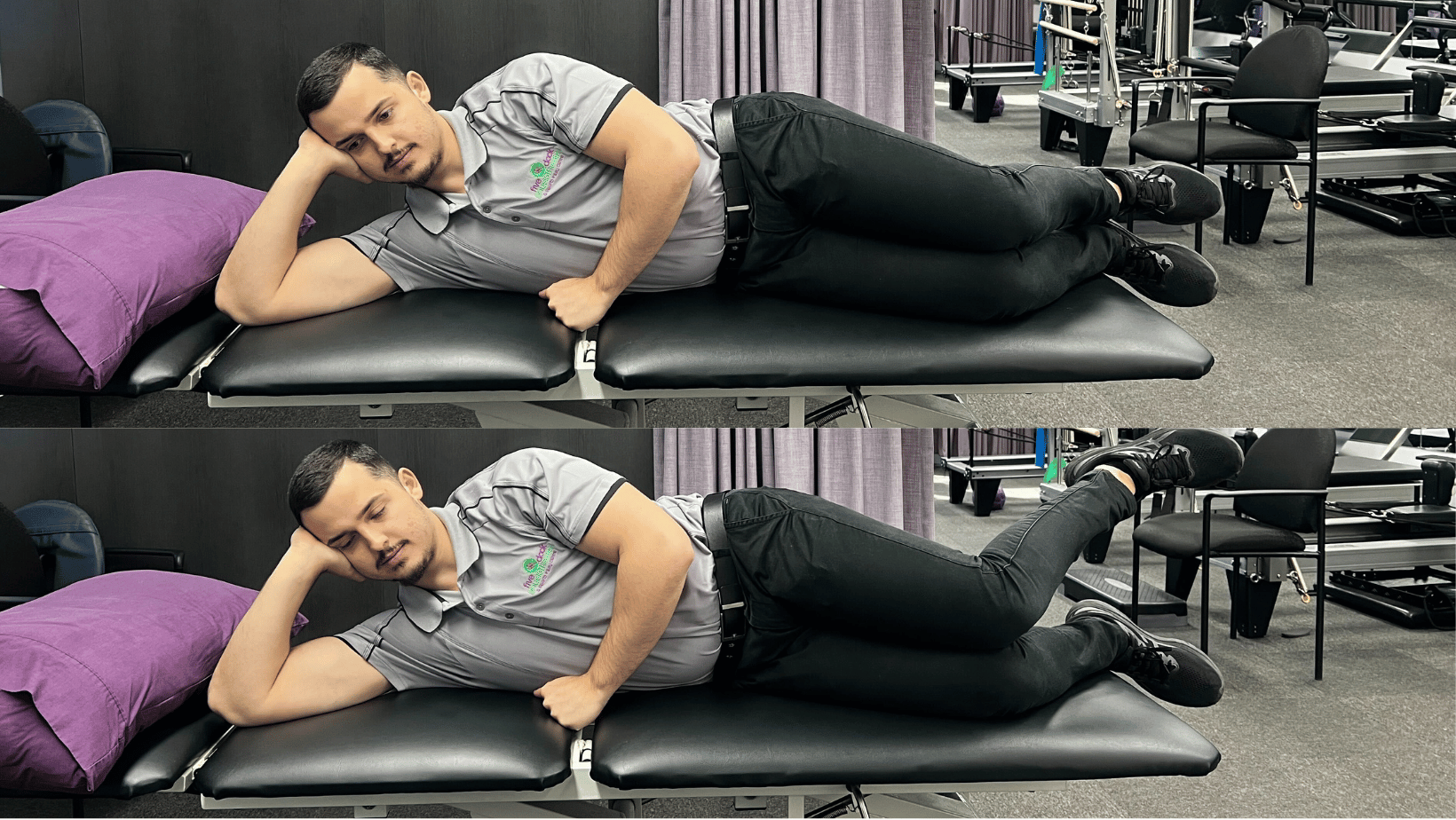
Side-Lying Hip Internal Rotation
Aim: Improve the deep hip stabiliser muscles
How: Lay on one side with knees bent to 90 degrees, and your feet, hips and shoulders in line. Engage your core muscles. Whilst your knees remain together lift your heels and hold for 5 seconds working your deep hip stabilisers. Repeat 10 times.
Improve lower limb strength primarily the gluteals, quadriceps, hamstrings and calf
Aim: Improve lower limb strength primarily the gluteals, quadriceps, hamstrings and calf
How: Stand in a split stance with your weight evenly distributed between the heel of your front foot (which is flat on the floor) and on your toes of the back leg. With your core engaged and your gluteals squeezed, lower yourself towards the ground allowing your back knee to bend, then return to standing. Repeat for reps.

If you or someone you care for has an injury, a flare up, requires some rehabilitation or experiences an increase in pain, give the clinic a call on 9713 2455 or book online.

