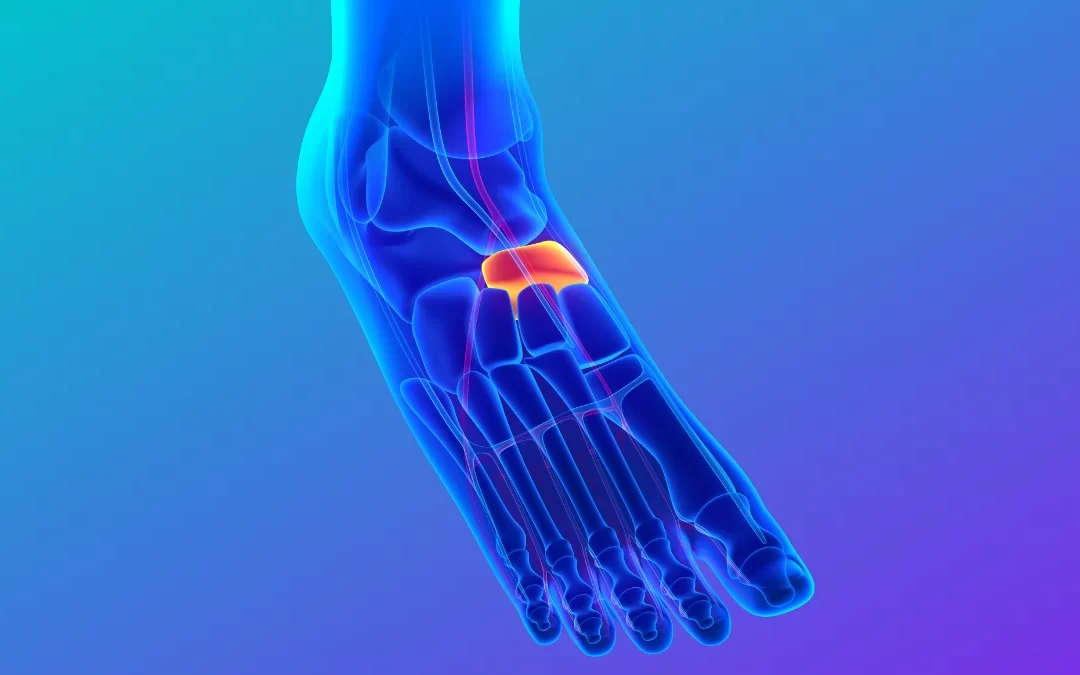
What causes a Navicular stress fracture?
The navicular, one of the 7 tarsal bones, is a bone located on the medial side or the inside of the foot. It provides stability to the arch of the foot and allows force to be transmitted for push off when walking. Navicular stress fractures are uncommon in the general population, however Potter et al., 2006 found that they accounted for 15% of all stress fractures. Mallee et al, (2015) found that they are more frequently present in younger athletes, especially males.
Navicular stress fractures are typically caused by repetitive stress to the bone, and it is widely accepted that the action of the Tibialis Posterior muscle which inserts into the navicular is a contributing factor. Continued chronic overuse or loading of the navicular subjects the cortex (outside layer) to weaken, resulting in microfractures and eventually a stress fracture.
Navicular Stress fractures are most commonly seen following periods of intense exercise without adequate rest or recovery and are common in athletes playing high intensity sports including running, soccer, basketball and dancing.

Symptoms
- Dull pain in the mid to top of the foot and radiate to the arch of the foot, especially during weight bearing activities.
- Tenderness on palpation of the navicular bone (The N spot)
- Initially patients will only have pain after high intensity activities or sporting activities but if not diagnosed or managed, pain can progress to low intensity activities such as walking, standing, and sitting.
- Possible swelling or bruising to the foot.
- Pain on resisted isometric testing of the tibialis posterior (inversion, plantarflexion)
- Altered foot mechanics.
Risk Factors
-
Intrinsic factors:
- Previous history of stress fracture
- Insufficient vascular supply
- Unfavourable foot/ankle biomechanics including excessive pronation or high arches.
- Low bone density
- Atypical foot structure, such as high arches
Extrinsic factors:
- Poor nutritional status
- Excessive/increase in training/exercise regime
- Inadequate footwear
Diagnosis and management of navicular stress fracture
Physiotherapists play a critical role in accurately diagnosing and managing navicular stress fractures. Diagnosis is typically made through a combination of clinical examinations and investigations such as x-ray or MRI to confirm the extent of the injury.
Depending on the severity of injury and the individual specific goals of the patient, surgical intervention may be required (Attia et al., 2021), however Torg et al, (2010) report that conservative management including physiotherapy should be considered the gold standard of care. Physiotherapy conservative management focuses on promoting bone healing, symptom management, restoring function and return to activity and sport. Orthotics or shoe modifications may be needed to provide additional support to the foot and prevent future injuries.
What does Conservative Management involve?
1. Rest and immobilisation: The first 6-8 weeks are usually immobilised in an orthopaedic CAM boot to remove stress from the fractured site and facilitate healing. Patients are typically non-weight bearing (NWB) for this period, so use crutches with evidence suggesting this to be the most important factor for recovery (Fowler et al., 2011). In this period pain management techniques such as ice therapy and soft tissue release are often required. The boot can be removed when the N-Spot is no longer tender (Brukner et al., 2018)
2. Manual Therapy Techniques: Brukner et al., 2018 also recommend that after the boot has been removed, it is essential for a physiotherapist to mobilise the stiff ankle, subtalar and midtarsal joints and provide soft tissue therapy to the calf, tibialis posterior and surrounding muscles followed by a progressive strengthening program.
3. Gradual return to weight-bearing activities: A gradual return to weight-bearing activities post immobilisation through a physiotherapy rehab program is vital to improve range of motion, muscle strength and stability, proprioception, and function. This is done through an individualised rehabilitation program centring around patient’s symptoms, weight-bearing activities, and introduction of specific functional tasks to promote healing and minimise the risk of re-injury (Romani et al., 2002). Gait retraining and biomechanical retraining are essential to correct compensatory patterns that may have led to the development of the stress fracture. Particular markers for recovery include improving tibialis posterior strength, calf strength, and pelvic/hip/knee control.
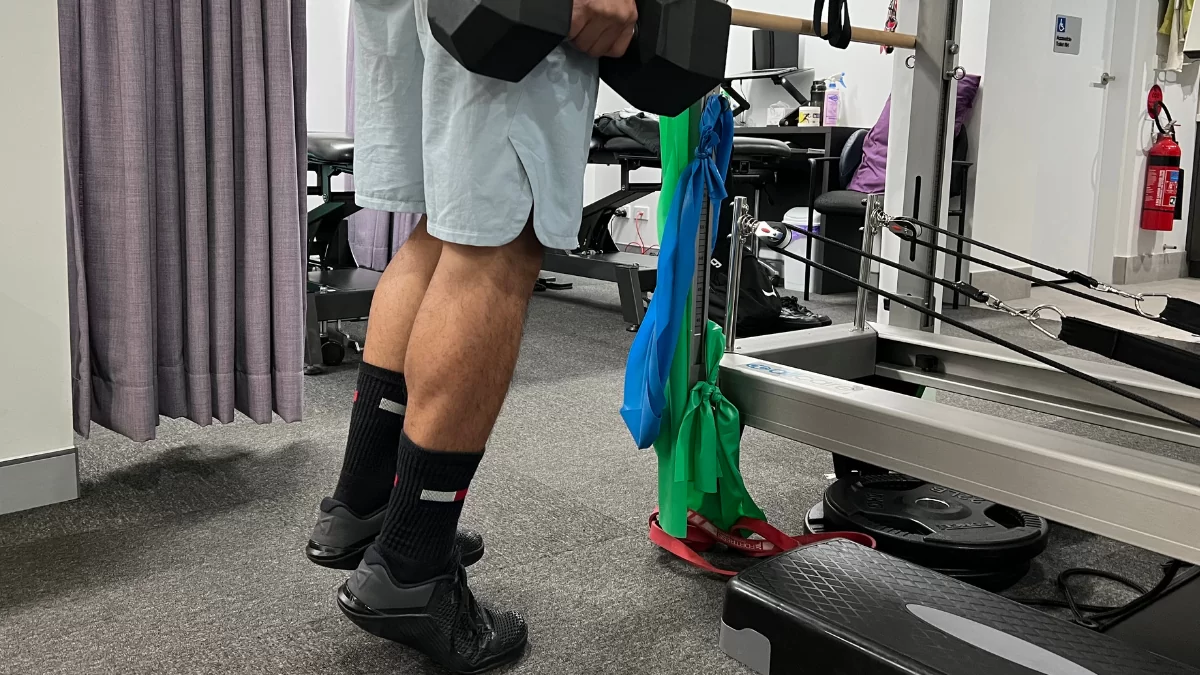
4. Return to activity or sport: Returning to physical activity too soon can increase the risk of re-injury. It is essential there is a gradual progression plan to return to high-intensity activities such as hopping, jumping, jogging, and running (Attia et al., 2021). Return to sport clearance is needed.
Things Physio’s use to assist with a Navicular Stress Fracture

CAM Boot
Our clinic stock both long and short CAM boots to suit most foot sizes – these are important to manage most foot and ankle fractures, high grade ligament injuries and tears of the plantar fascia and Achilles. They are integral in the recovery following a navicular stress fracture. Patients are required to wear a short CAM boot for 6-8 weeks to protect their injury and most protocols require Non-Weight Bearing in order for healing to occur. Our Physio’s are qualified to fit these CAM boots.
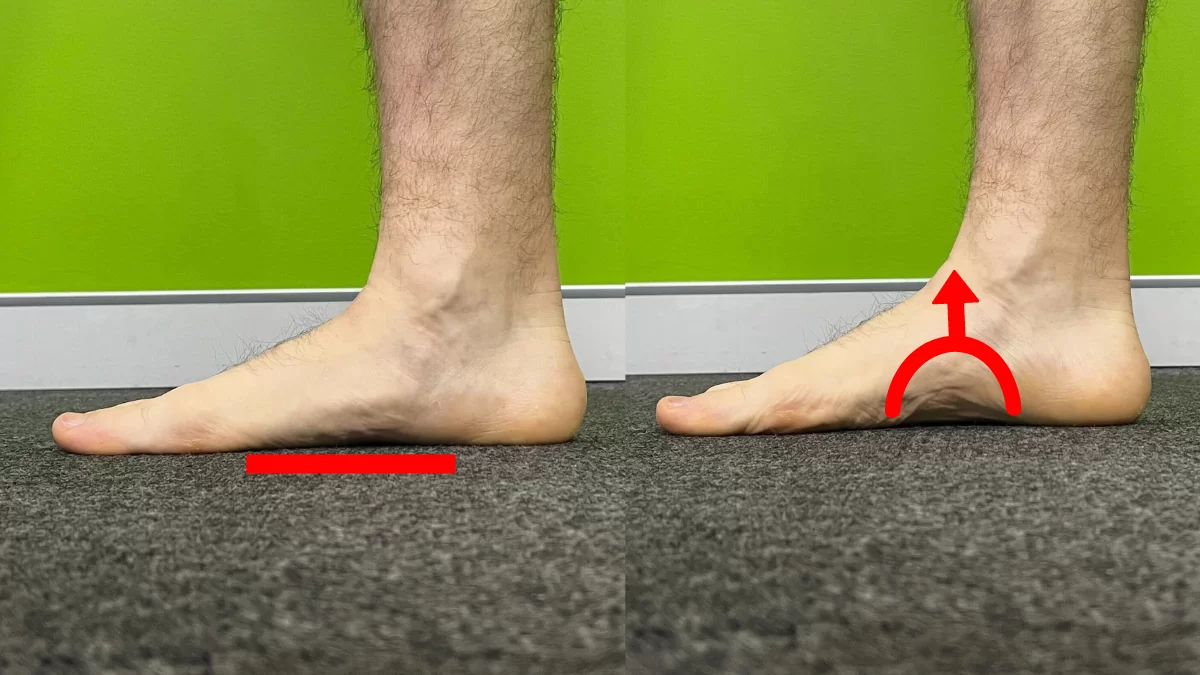
Tibialis Posterior Retraining – Arch Raises
Aim: Train the Tibialis Posterior muscle. This muscle runs up the inside of your shin and attaches to the navicular. It has an important role in helping to hold up your arch when weight bearing.
How do I do the exercise? In standing slightly roll onto the outside of your foot, lifting your arch half a centimetre up from the ground. Hold for 5 seconds before returning your foot to the ground and repeat for reps. This can be made more difficult by raising your arch and then going into a calf raise.

Wall Ball Single Leg Squat
Aim: Gluteus medius retraining. When your gluteus medius is activating well, it stabilises your pelvis and knee during a squat/single leg squat, making it less likely to let your knee buckle in. This in turn takes stress off the navicular and the bones on the inside of your foot.
How to do this exercise? Simply stand on the outside leg while simultaneously holding a ball onto the wall with opposite leg. Sit back into a mini 1-legged squat, training your gluteus medius muscle improving pelvic, hip and knee control and taking stress off the inside of your foot.