Do you get a sore knee when you walk up and down stairs or hills?
Does your knee niggle with squatting, sitting too much or when you stand up from sitting?
Does it hurt around your kneecap when you walk too much, run or jump?
If so you might be suffering from Patellofemoral pain syndrome (PFPS)
Patellofemoral Pain Syndrome (PFPS) is a common cause of knee pain seen in the general population, and largely experienced in those participating in sport and exercise. There has certainly been a rise in people complaining of PFPS with the increase in outdoor exercise during COVID lockdown as people look to walking and running for exercise and sanity. Unfortunately, PFPS can affect regular activities of daily living and can limit participation in exercise and organised sport. And the tough part is that research shows that 71-91% of patients with PFPS will experience continuous symptoms for up to 20 years following diagnosis unless this condition is treated (Rathleff et al., 2012), so it’s crucial that the underlying causes of PFPS are assessed and managed. The good news is that Alba-Martín et al. (2015) report that this is best achieved via physiotherapy assessment and rehabilitation.
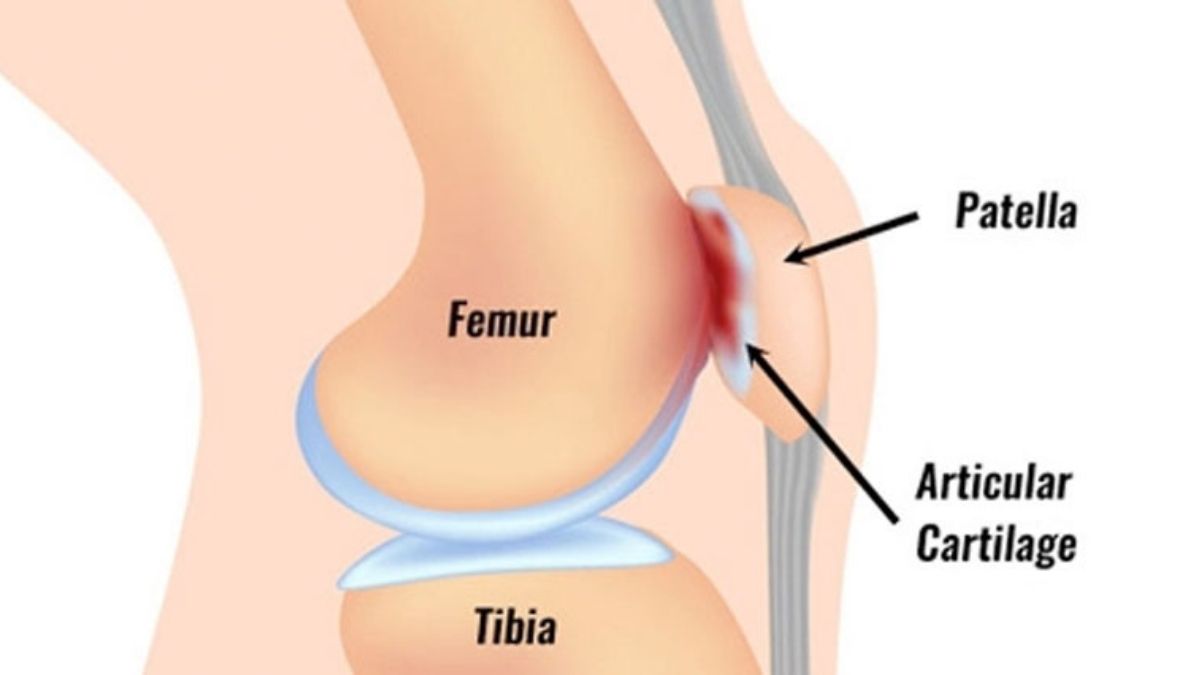
What Causes PFPS?
For regular pain free activity and optimal function of the knee, we require smooth tracking of the patella (kneecap) in its groove, the trochlear groove of the femur (upper leg bone). In patients with PFPS, normal movement of the patella is compromised or mal-tracking occurs. This may occur due to several factors, including muscle weakness or poor activation in the knee or hips, altered joint movement at the hip, knee or ankle: tightness in lateral structures of the hip and knee joint (ITB, vastus lateralis and lateral retinaculum) or poor neuromuscular control. The effects of abnormal kneecap tracking can be amplified with fatigue and an increase in load which may be due to training or incidental activity. Aggravating activities often include squatting, running, ascending/descending stairs or hills, prolonged sitting or jumping.
Patella alignment and its orientation is another cause PFPS (as the patella may glide or slide to one side more and thus cause overuse/overload on that part of the femur which can result in pain. In conjunction with this when the VMO (quads muscle on the inside of your knee) isn’t strong enough, the muscles on the outside can “win the tug of war that takes place” exerting a higher force and cause a lateral glide, tilt or rotation of the patella causing an overuse of the lateral side of the patella and result in pain or discomfort.
What are the biggest Risk Factors?
- A rapid increase in training or incidental volume or load
- Females are more at risk
- Previously unrehabilitated injury or poor compliance with post-operative rehabilitation
- Reduced gluteal and quadriceps strength or muscle activation
- Poor biomechanics
- Gastrocnemius and quadriceps tightness
- Pronated foot type
- Increased Q angle
How are symptoms described?
The most common symptom of PFPS is described as a dull, aching pain in the front of the knee or “behind the kneecap”. The onset of pain is often gradual, and activity related. Other common symptoms include:
- Pain during exercise and weight-bearing activities that involve repetitive knee flexion/extension, such as climbing stairs or walking downstairs, running, jumping, or squatting.
- Pain on the front of the knee after sitting for a long period of time with knee flexed.
- Clicking or crepitus in the knee during activities
- Usually, no true locking or giving way of the knee but can be reported as a result of muscle weakness or pain inhibition.
Diagnosis and Examination
Our physiotherapy examination is crucial in determining the root cause as well as contributing factors of PFPS. Thorough questioning by the physiotherapist will streamline the physical examination to help develop an appropriate management plan. Our physiotherapists will use specific tests and imaging where indicated to assess and exclude these other pathologies.
Identifying various intrinsic and extrinsic factors to the development of PFPS will guide the treatment plan. Simple things such as a change in footwear, an increase in load due to activity or an old injury or surgery that wasn’t properly rehabilitated can be critical bits of subjective information that can influence treatment and at times can help our physio’s suggest minor modifications that can help provide rapid relief of symptoms.
On our physio’s physical examination there are many different factors that may be observed contributing to or leading to PFPS including:
- Patella position, femoral position, and foot posture or position.
- Muscle size, activation and strength of gluteals, quadriceps, calf and core muscles.
- Presence of swelling
- Joint movement in the hip, knee and ankle
- Specifically an inability to straighten the knee (loss of extension) or pain with loaded knee flexion
- Pelvic position on single-leg stance and gluteal control (stability)
- Weak VMO activation (muscle on the inside of your knee that pulls the knee cap inwards)
- Muscle-length/tightness (hip flexors, hamstring, gastrocnemius, TFL, ITB)
- Walking/running technique
With the subjective history and the objective examination in mind, setting ideal functional goals when forming a treatment plan is critical to a good outcome as rehabilitation is guided by the activity levels those injured wish to return to and their current level of function.
How is PFPS treated?
The management of PFPS requires a comprehensive rehabilitation program that addresses all the underlying contributing factors. Symptom control is the initial aim of treatment, which includes load management, activity modification, exercise, ice, and patellar taping and bracing where indicated. Soft tissue and manual therapy will be used to address the tight tissue structures that lead to the abnormal tracking of the patella. Reduced patella mobility can be improved by using patella mobilisation techniques.
Load management is incredibly important to help reduce symptoms of PFPS. Load can be thought of as how much capacity or tolerance our muscles have in relation to activity. If we do more activity than our muscles can handle, fatigue sets in as does compensatory strategies (more stress on other muscles and joints), altered patellar tracking and often symptoms. Education around this and targeted exercise to improve our muscles capacity is integral to treating PFPS.
Pain-free exercise is essential when treating PFPS. Isometric exercises where the joints don’t move can be used initially with the knee fully straight as is this position the patella has no contact with femur, minimizing the stress through the joint. As rehabilitation progresses though, exercise selection is imperative. The prescription of closed kinetic chain exercises (CKC) or open kinetic chain (OKC) exercises is dependent on the patient’s capability and symptoms. CKC exercises are typically functional and provoke less stress through the PF joint so are almost always included in rehab (e.g. Squats). OKC exercises however are also important with Firoozkoohi Moghadam et al (2016) showing that OPC exercises had better results than CKC exercise when isolating quadriceps muscle contraction.
Our physios typically prescribe exercise programs focusing on improving quadriceps, core, gluteal and calf muscle strength, activation and stability, and proprioceptive exercises. This is governed by the deficits we see on assessment. Targeting the right muscles is imperative as pain causes muscle inhibition impacting our function and further leading to compensation strategies throughout our kinetic chain. As strength and function improves, and the exercise program is progressed, sport/task specific retraining can occur along with graduated return to activity. This may include a progressive running program, jumping or agility training where indicated. We aim to address all lower limb biomechanical deficits through the course of rehab to help reduce the likelihood of recurrent injuries. An ongoing program is typically recommended on discharge to help prevent recurrent issues.

What does the evidence say?
There is substantial evidence to support physiotherapy with Young et al, 2021 reporting reduced cost, improved outcomes, and reduced chance of recurrence of knee pain for patients who had physical therapy early compared to having delayed physical therapy. Although 17% of knee-related orthopaedic visits resulted in a diagnosis of PFPS (Willsey, 2018) the evidence strongly supports non-operative therapy with short-term use of NSAIDs, medially directed patella taping, and exercise programs targeting the lower extremity, hip, and trunk muscles. A research review in 2005 by Bolgla and Malone demonstrated good evidence regarding the use of exercise (vs passive modalities and stretching) for treatment of PFPS. Tyler et al. (2006) demonstrated very good results (93% of positive outcome measures) when hip strengthening is incorporated into PFPS treatment and Nakagawa et al. (2008) demonstrated additional benefits of combining strengthening at the hip and the knee when treating PFPS. Lower limb proprioception has also been shown to be lacking in patients suffering from PFPS (Akseki et al. 2008) and good results have been seen when incorporating specific proprioceptive training in rehabilitation (Clark et al. 2000). Mascal et al. (2003) noted that weakness of the hip, pelvis, and trunk musculature contributed to PFPS, thus this needed to be assessed and treated. Singh et al. (2019) found that patella taping could significantly engage the VMO and reduce PFPS, and there is also evidence for patellar braces and foot orthosis where indicated to help improve biomechanics and muscle activations (Petersen et al, 2014).
What’s the verdict?
Patellofemoral pain syndrome can be significantly improved with holistic physiotherapy rehabilitation, particularly when the treatment plan is designed individually for the patient, addressing their objective findings, it considers their activity levels and their goals.
Rehabilitation should gradually increase loading on the patellofemoral joint and surrounding tissues and address biomechanical deficits of all the muscles affecting the knee. A comprehensive biomechanical assessment will assist in determining muscle strength, motor control, flexibility and patella tracking. There is a risk of PFPS recurrence if an exercise program isn’t continued or adjustments to training routine and activity levels aren’t addressed.
GET AN ASSESSMENT & TREATMENT WITH OUR AMAZING PHYSIO TEAM.
- Get a crystal clear diagnosis on what’s causing your pain or injury
- Understand what activities you can do without suffering further consequences of knee pain and injury
- Commence rehabilitation improving your mobility and helping you get symptom free
- Set out a management plan so that you can achieve the best results
- Leave the session with the confidence of knowing exactly what to do to help you get pain free and back to sport, activity and full function

