The glenohumeral or shoulder joint is the most commonly dislocated joint in the body accounting for 50% of all major joint dislocations and unfortunately, shoulder dislocations make up the majority of traumatic sporting injuries.
But why does it dislocate so easily you ask?
Well, the shoulder joint is the most mobile joint in the body and is comprised of the articulation between the scapula (shoulder blade), humerus (upper arm bone) and clavicle (collar bone). The shoulder is one of the easiest joints to dislocate because the ball joint of the upper arm sits in a very shallow socket where it attaches to the shoulder blade. This makes the arm extremely mobile with the ability to move in many directions, but it also means that it is not very stable. Due to its high degree of mobility, the shoulder joint relies on both passive and active structures to supply stability whilst moving the arm.
The passive structures have the role of supporting the position of the joint and preventing the bones moving beyond their full movement capacity. These structures include the labrum (Cartilage lining), ligaments and joint capsule. Shoulder joint laxity or injury to any of these passive structures will lead to shoulder instability, which will increase the reliance on the active structures. The active structures (muscles) supporting the shoulder primarily consist of the rotator cuff muscles, which have the role of providing dynamic control to keep the ball stable in the socket as we move our arm or encounter impact.
Quite often, a shoulder dislocation can lead to secondary damage of these passive and/or active structures. A first-time dislocation can lead to a Bankart lesion in 82% of cases, which is damage to the labrum and/or glenoid bone (socket) or a Hills-Sachs lesion in 71% of cases, which is damage to the head of humerus (ball).
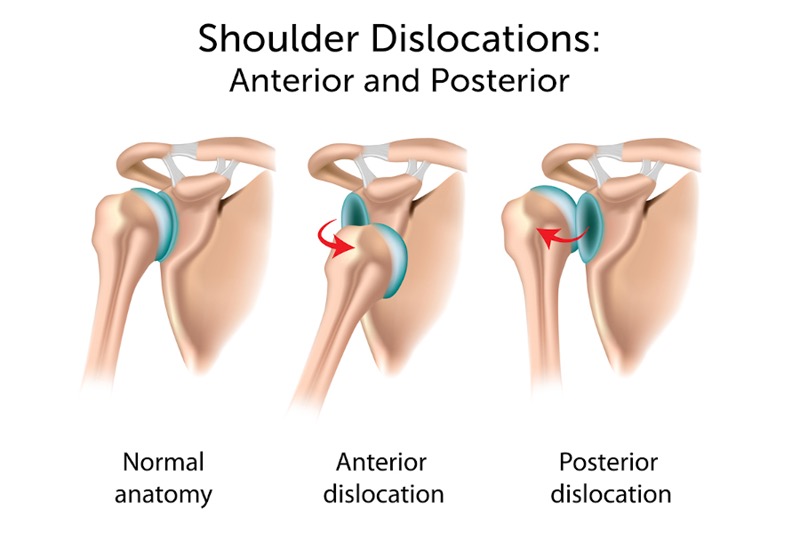
Does a shoulder always dislocate the same way?
No, the shoulder can dislocate in 3 common ways. The most common is when the humerus pops forward. This is called anterior dislocation and occurs in 95-97% of cases (Sherman, 2019). The most common instance for young people is sports related trauma and for the elderly, a fall on an outstretched arm. The other common way the shoulder is dislocated is posteriorly, where the humerus (arm bone) pops backwards behind the shoulder. The rarest kind of dislocation is an inferior dislocation. Generally, this is caused by something/someone pushing the arm downwards.
What is the difference between a subluxation and dislocation?
People will “sublux” their shoulder which is different to a dislocation. A subluxation is an incomplete or partial dislocation where the ball of the arm bone does not completely come out of the shoulder socket. This can happen in one of the ways mentioned above, however the shoulder will not be required to be “popped” back in. Although this is not as severe as a dislocation, it is important to have the shoulder assessed and treated by a physiotherapist in order to address the underlying factors resulting in the shoulder instability. This will prevent further subluxation, further damage to the other structures in the shoulder like the muscles or potential dislocation in the future.
What to do if you suffer a dislocation?
1. Seek immediate medical care
If the shoulder hasn’t popped back in, it is important that a professional performs this in a quick and safe manner to avoid secondary damage to the shoulder. If not done correctly, nerve damage and further trauma can occur, so this is vital. It is then advised that scans are performed to assess the surrounding structures.
2. Scans
An X-ray should always be performed to ensure the shoulder is positioned correctly after being relocated as well as to rule out bone damage.
If there is severe weakness or heavy bruising, an MRI may be required to rule out soft tissue damage to the muscles and passive structures of the shoulder like the labrum.
3. Immobilisation
After being relocated, the shoulder should be kept in a sling for a time period determined by your doctor and physiotherapist. Current evidence varies, but a 2–4-week period is the common recommendation.
4. Physiotherapy rehabilitation
Physiotherapy should begin after the immobilisation period to ensure you are able to regain shoulder movement and control. This will help reduce the risk of secondary complications including frozen shoulder and help reduce the chance of further instability.

What is the role of physiotherapy?
As mentioned, the shoulder needs to be relocated as soon as possible by a professional and followed up with an X-ray/MRI and placed in a sling as suggested above. Our physiotherapists can then provide a thorough assessment to determine if further imaging (MRI) and specialist referral is required. Orthopaedic referral is indicated if instability is found on testing, or if a Hills Sachs or Bankart injury is found.
Early physiotherapy helps to reduce pain, encourage movement, and prevent compensatory movement patterns whilst beginning rehabilitation either with non-operative conservative management or in preparation for surgery. Initially, this will include activating the appropriate muscles around the shoulder blade and shoulder joint to provide the shoulder with stability and control. This will progress to strengthening of the rotator cuff muscles and strengthening of the shoulder in general, improving shoulder blade control through movement and will include more challenging exercises as rehabilitation progresses further. This will typically involve training movements above the head and with weight, helping patients get back to their normal activities of daily living or their sport specific functional activities in order to return to sport or their previous capacity once appropriate.
Completing a comprehensive rehab program is essential for the safe return to sport and prevention of subsequent dislocations. It will also help to minimise subsequent surgery, arthritis, and poor functional capacity (both in conservative and surgically managed patients). Other important considerations are the effects of the kinetic chain on the shoulder, and thus biomechanics and lower limb kinematics are assessed in our clinic and holistic strengthening programs are prescribed where indicated.

Current evidence
Re-injury risk
Hovelius et al 2008 in a 25-year study found that 72% of 12–22-year-olds, 56% of 23–29-year-olds and 27% of 30 years+ suffered subsequent dislocations after non-operative management.
Initial management & immobilisation
Current evidence and guidelines support shoulder reduction as soon as possible followed by sling immobilisation. In a younger population Paterson et al 2010 found no benefit of sling immobilisation greater than one week, whilst Shin et al 2012 supports a 2–4-week period of immobilisation for patients over 60 years old.
Management
Jakobsen et al 2013 compared conservative management alone versus surgery plus rehab in first time traumatic dislocations. At 2-year follow-up, 54% of conservatively managed patients had recurrent instability compared to 3% in the surgery and rehab group. However, when deciding on management, Sachs et al 2011 states the strongest predictors to recurrent instability need to be considered; under 25 years, participation in contact sports, using arm above chest for occupation. It is important to remember conservative management is progressively more successful with age with Rehabil et al 2017 outlining a 6-week rehab protocol to attain full movement and strength compared to the unaffected side making physio rehab an essential component of recovery.
So what are the take away points?
- Shoulder dislocations can be a debilitating and painful occurrence that can affect the function of the shoulder – after encountering a shoulder dislocation, it needs to be relocated urgently and then assessed thoroughly by a professional.
- It’s best to involve a physiotherapist early in the process to conduct an assessment, and help decide whether surgical opinion is required, and they can also begin early treatment regardless of whether surgical management will be required or not. After the immobilisation period the physiotherapist will help plan the recovery in order to improve function and get people back to doing the activities they love.
- Physiotherapy is an essential component in rehabilitation, with Rehabil et al (2017) finding that a 6-week rehabilitation protocol assisted in regaining full shoulder range of motion and strength in the injured shoulder.

Do you have shoulder pain or instability that’s impacting your life?
GET AN ASSESSMENT & TREATMENT WITH OUR AMAZING TEAM OF PHYSIO’S.
- Get crystal clear about what’s causing your shoulder issue
- Understand what activities you can do without suffering consequences of shoulder pain or instability
- Find out the simple yet essential exercises that can help you achieve amazing result
- Leave the session with the confidence of knowing exactly what to do to get symptom free and back to living life to the full

