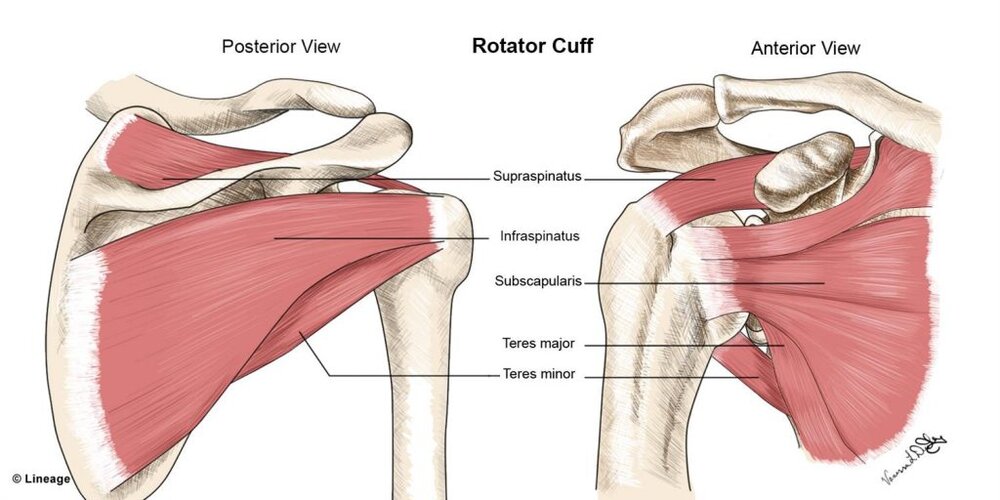
The Rotator Cuff (RC) is comprised of 4 muscles and their tendons: Supraspinatus, Infraspinatus, Subscapularis and Teres Minor.
The shoulder is the most mobile joint in the entire body making it easily susceptible to injury. Therefore, it requires a high degree of strength, stability and control which is provided by the RC muscles. RC Tears can either be traumatic or as a result of degeneration occurring in both sports people and the general public.
In a review by Mingawa et al. (2013), they found that the prevalence of rotator cuff tears in the general population was around 22%, which increased with age, and interestingly an asymptomatic tear was twice as common as symptomatic tear on imaging.
Causes
Rotator cuff tears can be separated into two categories:
Traumatic: A one off incident as a result of a fall or external force. This can be associated with a weakened or fatigued muscle being overloaded, leading to a tendon rupture.
Degenerative: A result of gradual degeneration of the tendon due to overuse, poor biomechanics and age. These tears can have an insidious onset of pain and are usually exacerbated by movement. Rotator cuff tendinopathy often proceeds a tear as it is associated with tendon degeneration creating pain and weakness.

Risk Factors
- Age: full-thickness rotator cuff tears present in approximately 25% of individuals in their 60’s, and more than 50% of those in their 80’s.
- Those who participate in contact and throwing sports
- Overuse or repetitious above head tasks
- A history of shoulder arthritis
- Poor biomechanics – including lower kinetic chain dysfunction
Signs & Symptoms
- The most common signs of rotator cuff injuries are:
- Pain at rest and at night, particularly if lying on the affected side.
- Pain when lifting and lowering the arm or with reaching.
- Pain during ADL’s like dressing, doing hair and domestic activities such as scrubbing and hanging laundry.
- Weakness when lifting or rotating the arm.
Imaging
The most common and accurate imaging method to evaluate rotator cuff pathology is MRI. It can detect tears and inflammation and may help to determine size and character of the tear in order to establish what appropriate treatment might look like. Although MRI is the gold standard imaging method for rotator cuff pathologies, diagnostic ultrasound can also be used as it has a good diagnostic accuracy in the hands of a good sonographer, so can be more cost effective and readily available.

Findings on Assessment
- Pain typically localized to anterior/lateral region of the shoulder, and may refer down the lateral upper arm.
- Painful & restricted range of motion into flexion, abduction and internal rotation.
- Muscle weakness & pain on manual muscle testing (typically abduction, ER & positive special tests like the empty can test)
- Functional impairments: difficulty lifting, pushing, reaching, overhead movements and moving the hand behind the back (IR).
- Scapular Dysfunction. Studies of patients with rotator cuff tears have shown increased scapular upward rotation of some magnitude (Kibler et al. 2013).
Surgery vs Conservative Management
Historically partial RC tears have been treated with surgical repair and subsequent rehabilitation due to the inability of the tendon to repair independently.
Recent evidence however, advocates for conservative rehabilitation as the initial treatment modality with Ryosa et al., (2017) demonstrating that surgery is not more effective than conservative rehabilitation alone in partial thickness tears.
Jeanfavre et al., (2018) further emphasised the benefit of exercise therapy with pain, range of motion, strength and function all improving in greater than 80% of participants, with only 15% of RC tears transitioning to surgery. Abdulwahab et al., (2017) reported “a conservative treatment program is a reasonable approach within the first 6–12 weeks in patients with non-traumatic tears. If the patient does not respond within the initial 4–6 weeks, then it can be an indicator for transition to surgical treatment.”
If, however, the RC tear is moderate to large or the functional deficit is significant then surgery may be required more urgently. The most common rotator cuff muscle that is torn is the supraspinatus tendon and it is normally repaired via arthroscopy. Following surgery there is typically a period of immobilisation before post-op physiotherapy and rehabilitation can begin guided by the surgeon’s protocol. Thomson et al. (2016) conducted a study into post surgical protocols and found that post surgical improvements were achieved consistently across varying rehab protocols.
How Does Physiotherapy Help?
Once a tear is confirmed, a decision regarding conservative or surgical management needs to be made based on the severity of the tear, age of the patient, objective measures seen on examination and their functional and sporting requirements and goals. Physiotherapy aims to achieve full range of motion, improve scapular control and restoration of strength, motor control and flexibility with a graded return to full activities/sport/function.
At Five Dock Physiotherapy & Sports Injury Centre we provide both manual therapy when indicated alongside individualised and progressive exercise programs for our patients that focus on improving strength, endurance and motor control through full shoulder motion. This takes into consideration scapular mechanics and the kinetic chain to achieve optimal results. Kinetic chain exercises may include lower limb strengthening, core and gluteal exercises and mobility work to improve thoracic, cervical or lumbar ROM and often progress to functional and task specific exercises. The impacts of posture, education around its impacts and postural retraining exercises are also included where needed.
In our clinic we also use the AxIT system as part of our management. The AxIT system uses force plates and dynamometers to assess strength, endurance and power of specific muscle groups. It allows us to identify muscle imbalances side to side in the rotator cuff and also analyse the body’s ability to produce force by testing other areas in the kinetic chain. This data can help guide our patients during conservative management or post-op rehab giving them realistic measures and goals to a achieve as they return to function.


