Often referred to as a high ankle sprain, “syndesmotic injuries, account for around 11% to 17% of total ankle sprains” (Salaameh et al, 2022). The Sydnesmosis is a complex ligamentous structure that joins the tibia and fibula just above the talus of the ankle. It is critical that injuries to the syndesmosis are diagnosed correctly as the management and prognosis of this condition can vary considerably to that of the more common lateral ligament sprain, and if misdiagnosed or mismanaged they can lead to “Functional limitation from instability, and chronic pain secondary to joint degeneration”. (Inge et al., 2015)
The syndesmosis provides stability for the articulation of the tibia and fibula. The anterior syndesmosis consists of the anterior-inferior tibiofibular ligament (AITFL), the middle part is attached by the interosseous ligament (IOL), the posterior syndesmosis includes the posterior-inferior tibiofibular ligament (PITFL), and the transverse tibiofibular ligament (TTFL).
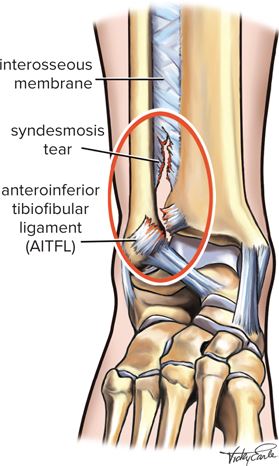
Cause of Injury
Syndesmosis injuries are most commonly a result of excessive ankle external rotation combined with axial loading of the ankle. Alternatively, they may also be sustained with an isolated hyperdorsiflexion of the ankle. These positions lead to a forceful widening of the ankle mortise, tearing the AITFL and separating the fibula from the tibia. Increased severity and force can tear the deltoid ligament, PITFL and interosseous ligament and can cause a fibula fracture (Maisonneuve Fracture) leading to pronounced instability. These injuries have a higher occurrence among athletes that play contact sports involving fast changes in direction, twisting or cutting manoeuvres such as football, rugby and basketball.
Diagnosis and examination
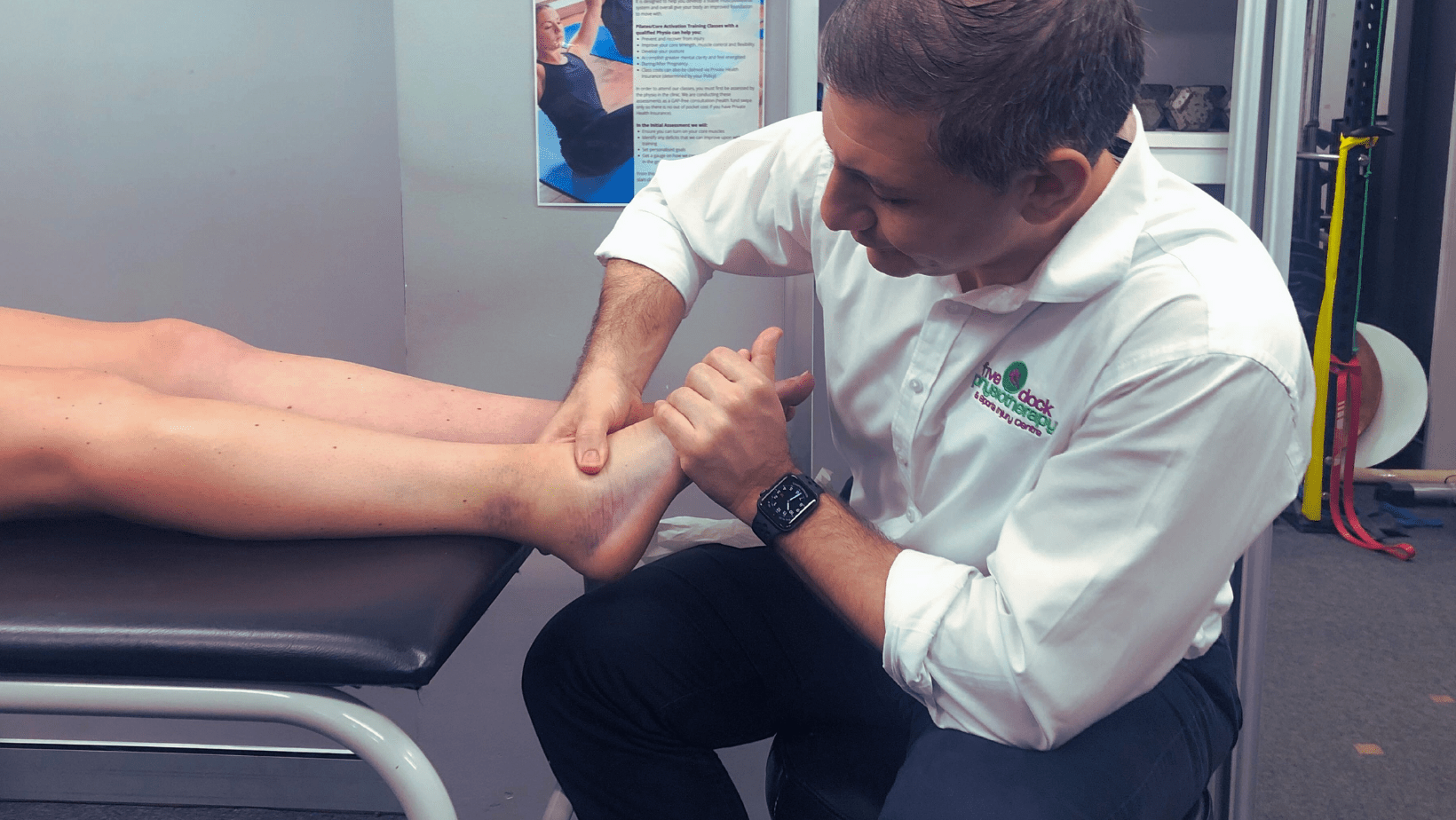
Physio diagnosis involves a thorough subjective and objective assessment. Common clinical features
are present on assessment:
- Reduced power at push-off, calf weakness and reduced ability to weight bear
- Tenderness over the AITFL, IOL or any of the mentioned ligaments
- A positive external rotation and dorsiflexion stress test
- A positive squeeze test
- Swelling
Once a syndesmosis injury is suspected, a CAM boot and crutches are typically organised for the
patient and they are referred for a weight bearing x-ray followed by an MRI to confirm diagnosis and
assess the severity of the injury.
Surgery or Conservative Physio Management?
With unstable injuries to the syndesmosis, patients potentially require internal fixation surgery to prevent further instability and injury to the joint. The amount of instability present on examination and the severity of injury found on MRI are the main factors that indicate whether surgery is required. In our clinic we have a good relationship with a number of orthopaedic surgeons that will happily give us guidance with these injuries as misdiagnosing an unstable syndesmosis injury correlates with poor outcomes. These patients are typically referred to the surgeon who determines whether surgical or conservative management is required.
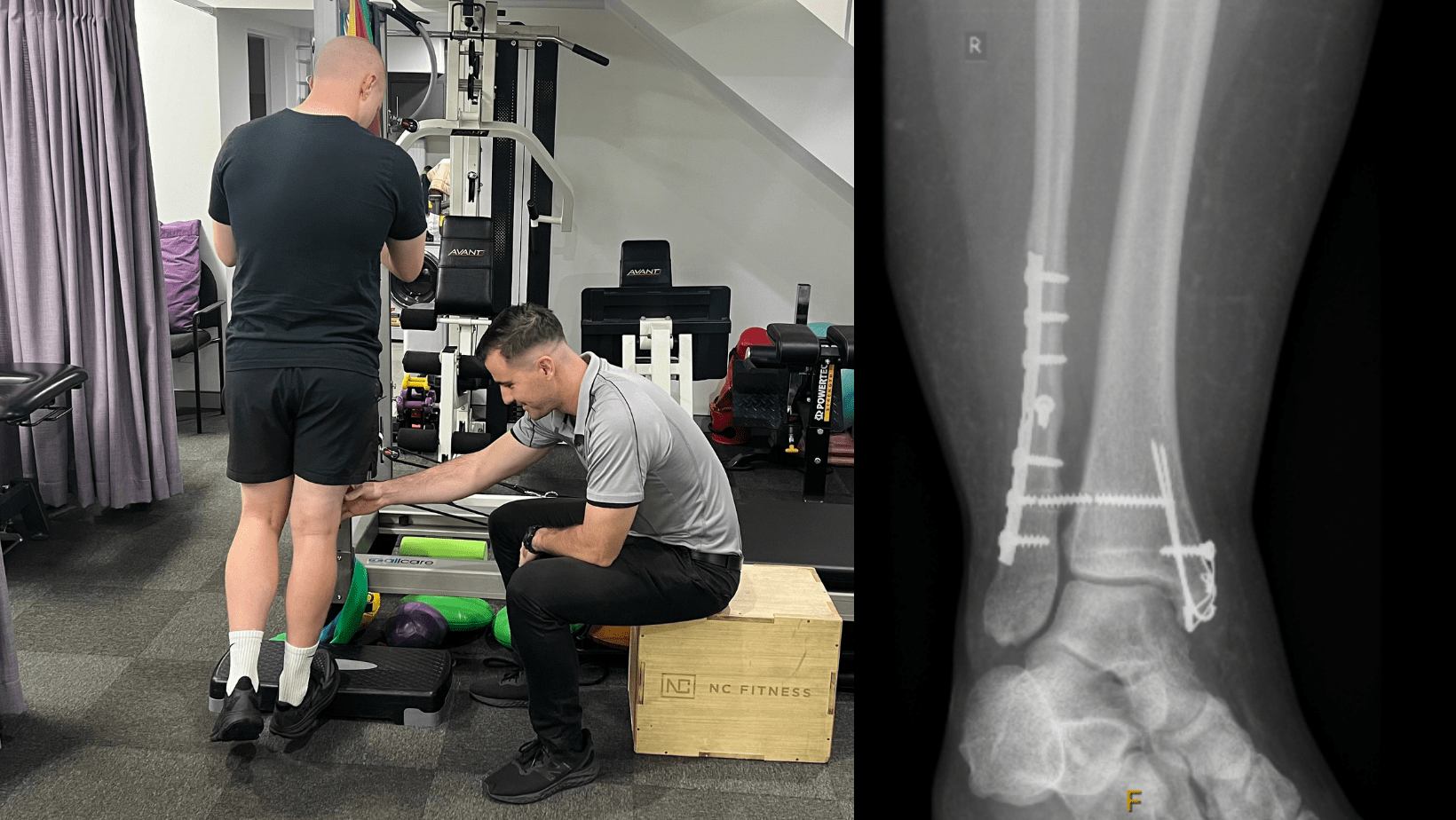
Physio Rehab
Rehabilitation can start on day 1 post-injury if a fracture is not suspected (or is cleared by x-ray). The first phase in rehabilitation focuses on promoting healing to protect the joint thus a CAM boot is typically provided. This phase of treatment also aims to reduce inflammation and maintain ankle mobility while integrating safe (typically non-weight bearing) strengthening. Ice and compression are used in this phase, as is manual therapy.
Research indicates this period of immobilisation should be followed by a gradual and staged rehabilitation and return to sport program to reduce the risk of re-injury and development of premature ankle arthritis which occurs in 40% of unstable syndesmotic injuries (D’Hooghe P, et al 2020).
The second phase concentrates on normalising ROM (range of motion) and gait, regaining strength throughout the lower limb and aiding a return to normal activities of daily living. This stage is primarily focused on addressing any movement compensations that have occurred from walking with a limp or being immobilised in the CAM boot, thus it addresses the entire kinetic chain. Furthermore, this subacute phase of rehabilitation includes balance and proprioception training helping to reduce the risk of re-injury in the future.
Manual therapy, including soft tissue work and mobilisations, play an important role in gaining symptom relief, restoring ankle ROM and managing muscle compensations throughout early rehabilitation.
The third phase of rehab occurs when the patient is able to jog and hop on the injured ankle without pain or instability (Williams & Allen 2010). This phase incudes agility training, plyometric work, jumping and running retraining. A safe return to sports requires the player to perform sports specific tasks and participate in full training and contact at actual game speed with quality movement and minimal discomfort (Williams & Adams 2010).
An accurate diagnosis is integral to successful management and prognosis of any syndesmosis injury. Poor rehabilitation even in low grade injuries results in 30-70% of patients reporting persistent pain, ongoing time away from work and sport and also results in impairments in activities of daily living. With no rehabilitation or poor management, these ongoing limitations can range from 6 months to seven years post injury (Brison et al, 2016). Conversely, the comprehensive rehabilitation of a syndesmosis injury leads to a reduced chance of developing ankle arthritis in later life. It is important to note thatrehabilitation of a syndesmosis injury can take up to twice as long as a normal lateral ankle sprain. (Van Dijk CN et al. 2016).
Exercise
Wobble board Circles
Aim: Improve balance and proprioception
How: Stand on a wobble board with feet shoulder width apart. Shift your weight along the outside edge, with weight going from ball to heel of your foot right to left so that you move in a circular motion. Reapeat 10 times each way training your balance and your ankle muscles through the extremities of movment.

Banded Self Mobilisation
Aim: To improve ankle dorsiflexion range of motion
How: Loop a theraband or powerband around a stationary surface and around your distal tibia of the affected ankle close to the joint. Place your affected foot on a box and simply drive your knee forward, actively dorsiflexing your ankle. The resistance band applies a traction to the tibia, enabling your ankle to dorsiflex more easily, serving a self mobilisation. Hold 3 secounds. Repeat 10 times

If you or someone you care for has an injury, a flare up, requires some rehabilitation or experiences an increase in pain, give the clinic a call on 9713 2455 or book online.

