Patellofemoral Pain Syndrome (PFPS) is a common cause of knee pain seen in the general population, and largely experienced in those participating in sport and exercise. The most common symptom of PFPS is pain occurring at the front/inside of the knee during loaded knee flexion positions such as walking upstairs/downstairs, prolonged sitting, squatting, running, or jumping.
For regular pain free activity and optimal function of the knee, we require smooth tracking of the patella (knee cap) in its groove, the trochlear groove of the femur (upper leg bone).In patients with PFPS, normal movement of the patella is compromised or mal-tracking occurs.
Causes
PFPS may occur due to a number of factors, including weakness or poor activation of the muscles around the knee or hips, altered joint movement at the hip, knee or ankle; tightness in lateral structures of the hip and knee joint (ITB, vastus lateralis and lateral retinaculum) or poor neuromuscular control. The effects of abnormal knee cap tracking can be amplified with fatigue and an increase in overall load which may be due to training or incidental activity.
Patella alignment and the patella’s orientation are another cause of PFPS as the patella may glide or slide to one side more as it tracks in its groove and cause overuse/overload on that part of the femur which can result in pain.

Risk Factors:
• A rapid increase in training or incidental volume or load
• Reduced gluteal and quadriceps strength or muscle activation
• Poor biomechanics
• Gastrocnemius and quadriceps tightness
• Pronated foot type and increased Q angle
• Previously unrehabilitated injury or poor compliance with post-operative rehabilitation
Treatment and evidence:
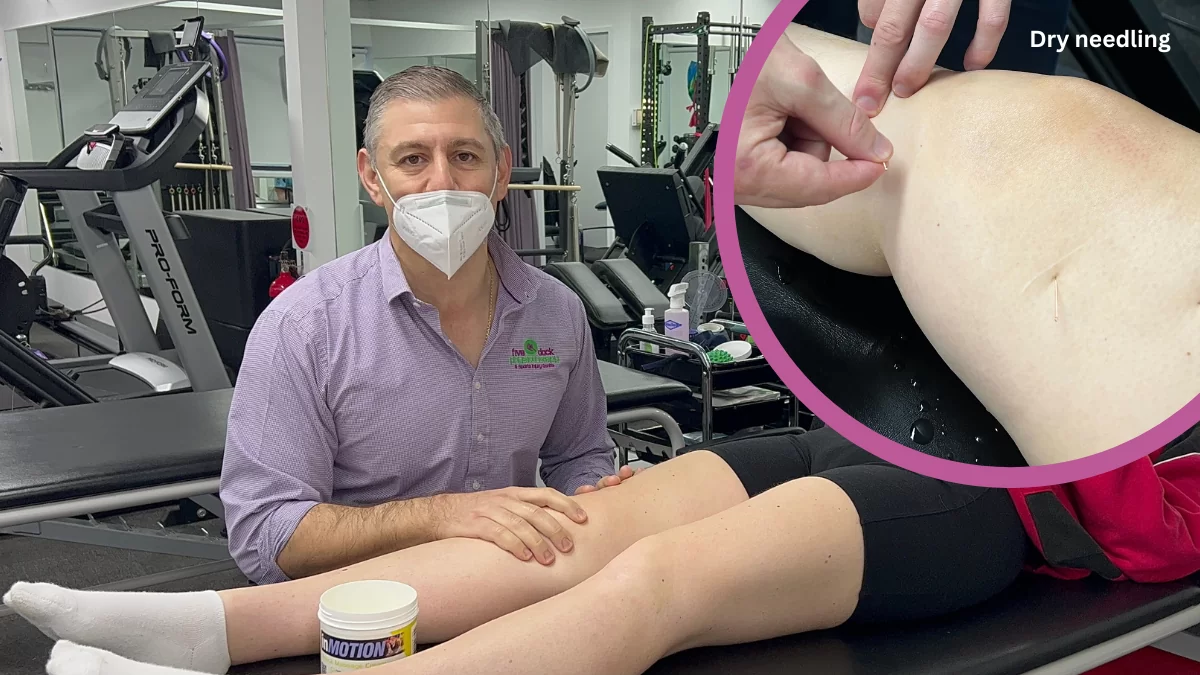
The management of PFPS requires a comprehensive rehabilitation program that addresses all the underlying contributing factors noted on assessment. Symptom control is the initial aim of our physio’s treatment, which includes; load management, activity modification, exercise, ice, and patellar taping and bracing where indicated. Soft tissue and manual therapy will be used to address the tight tissue structures that lead to the abnormal tracking of the patella. Improved patella mobility can be facilitated by using patella mobilisation techniques.
There is strong evidence to support the use of exercise programs focusing on addressing the biomechanical causes of the symptoms, namely improving quadriceps, core, gluteal and calf muscle strength, activation and stability, and proprioceptive exercises. Tyler et al. (2006) demonstrated very good results (93% of positive outcome measures) when hip strengthening is incorporated into PFPS treatment and Nakagawa et al. (2008) demonstrated the benefits of combining strengthening of the hip and the knee muscles when treating PFPS.
Targeting the right muscles with an exercise program is imperative as pain causes muscle inhibition impacting our function and further leading to compensation strategies throughout our kinetic chain. As strength and function improves, and the exercise program is progressed, sport/task specific retraining can occur along with graduated return to activity. This may include a gym program and a progressive running program, jumping or agility training where indicated. We aim to address all lower limb biomechanical deficits through the course of rehab to help reduce the likelihood of recurrent injuries.

Exercises to help Achilles tendinopathy.
Static Lunge
Aim: It is a dynamic exercise that works many of our lower limb muscles through range of motion. Improves gluteal stability, calf stability, core strength, hamstring stability and quadricep strength (particularly the Rectus Femoris).
How do I do the exercise: Stand in a split stance with one leg forward and one back. You’ll need to be up on the toes of your back leg and have your weight on the heel of the front leg. There’ll be a slight bend in both knees to start. Once you’ve engaged your core muscles and tensed your gluteal muscles of the back leg, you’re ready to go. From there lower yourself straight down allowing both knees to bend, whilst staying up on your toes of the back leg and keeping your glutes engaged the whole time. Lower the back knee to a 90 degree angle, then press up to start position and repeat.

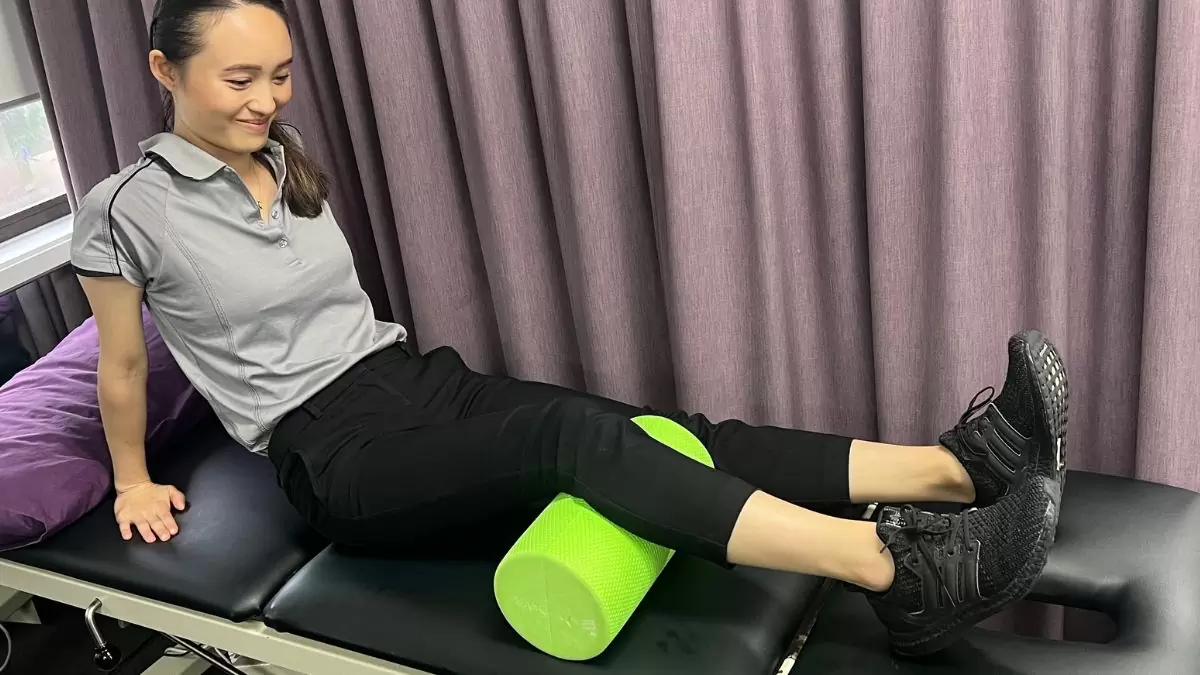
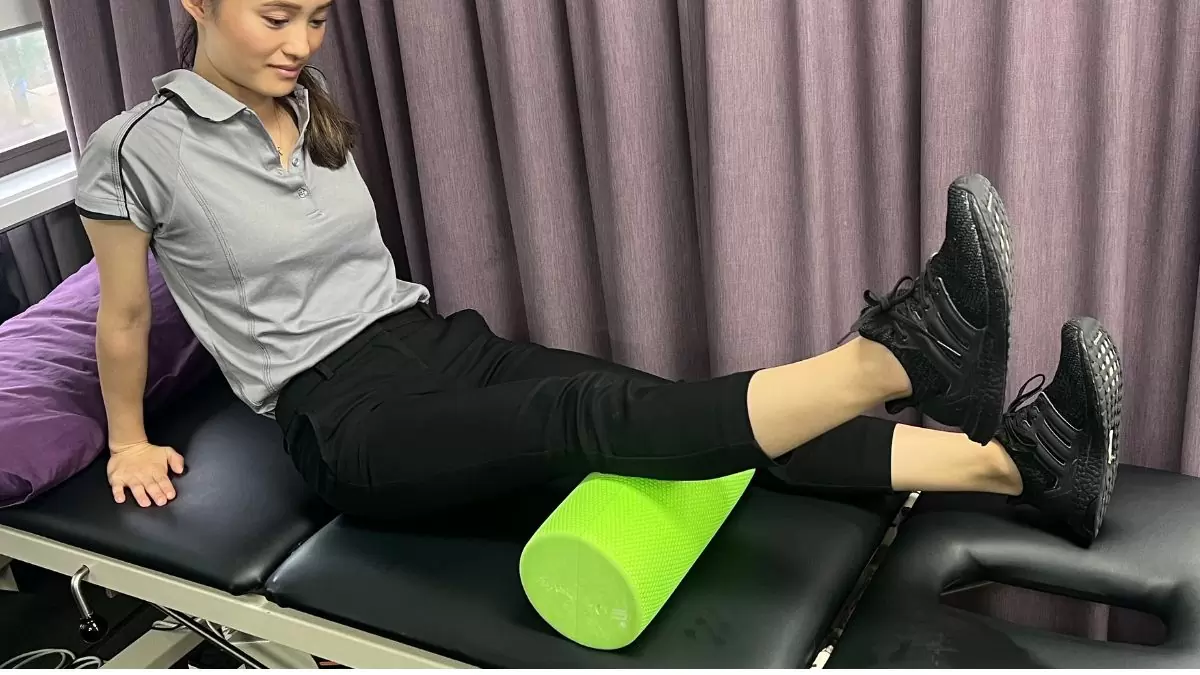
Foam roller the ITB (Iliotibial band)
Aim: Reduce muscle overactivity in the ITB which attaches to the outside of the knee. When overactive, the ITB pulls the kneecap laterally (to the outside) and causes patella mal-tracking. This overactivity often occurs when there is gluteus medius weakness.
How do I do the exercise: Lie on your side with the roller perpendicular to the outside of the thigh below the hip joint. Support your body weight and hold yourself up using the arm closest to the ground and also place weight through the top leg having it bent in front of you. Keep the leg you’re about to roll on straight, then simply roll back and forth (never going lower than your knee) massaging the area to reduce tightness and overactivity, thus taking stress off the ITB, and consequently the knee.

Inner Range Quad
Aim: To improve activation and strength of the VMO (Vastus Medialis Obliques), the muscle that pulls your patella or kneecap medially allowing it to track in its grove. This muscle is critical in the last 30⁰ of knee extension, so very important up and down stairs, when squatting and when straightening the leg all the way. In PFPS this muscle is often inhibited by pain or can lack endurance.
How do I do the exercise: Place a rolled up towel or a roller under your knee crease. Simply kick out, extending your knee straight, tensing the muscle on the inside of your knee. Hold for 5 seconds and repeat 10 times. Level of difficulty can be increased by increasing reps, hold time, going through full movement or by adding weight. It will often be progressed into a more functional exercise.