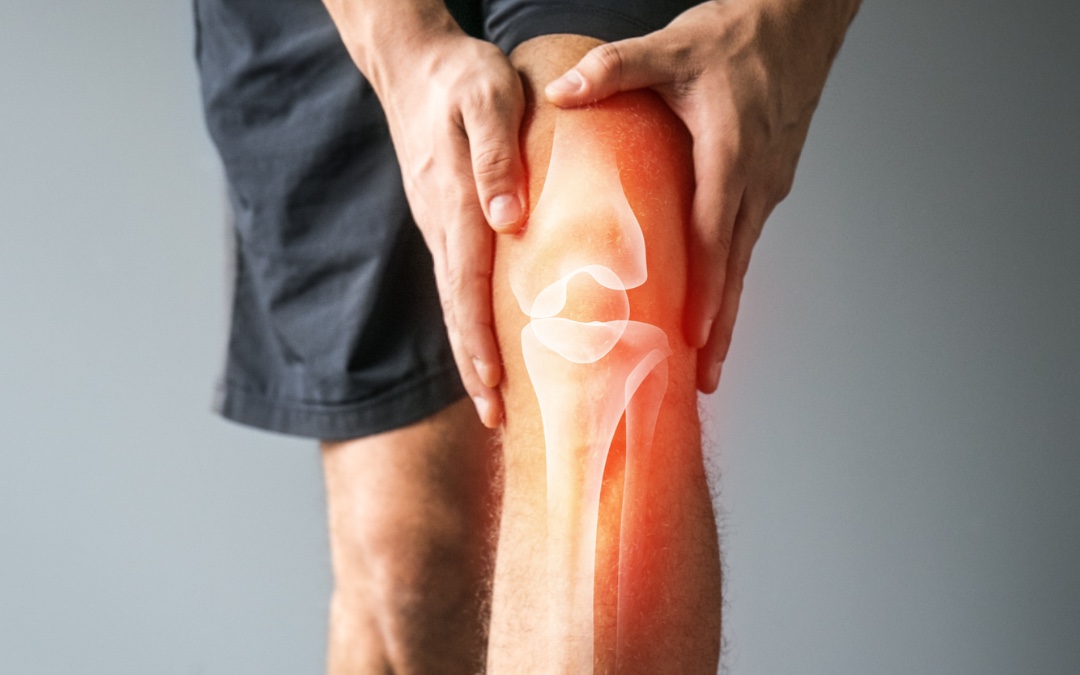
The medial and lateral menisci are two C-shaped fibrocartilaginous structures found on the boney surfaces of the knee. They act as a shock absorber, help stabilise the knee and are an attachment site for tendons, muscles and ligaments.
How is the meniscus injured?
An acute meniscus tear usually occurs with weight bearing and twisting mechanisms, commonly involving a change of direction or landing awkwardly. There are other types of meniscus tears that are degenerative in nature and usually present with an increase in age or “wear and tear”.
Risk Factors
- Sports involving twisting/pivoting, jumping and landing—netball, soccer, volleyball, basketball
- Contact sports—AFL, rugby,
- Inherent ligamentous laxity
- Previous knee injury—MCL, ACL
- Increasing age

Examination and Diagnosis
When examining the knee, the subjective history or questioning is important in determining which structures of the knee may be potentially injured. With a meniscal injury, the mechanism of injury will usually be one associated with pivoting, twisting, or changing directions. The individual may present with symptoms of clicking, catching, locking, or giving way of the knee. Alternatively, in a degenerative meniscus, symptoms may present slowly over time without a significant event. Aggravating factors can include prolonged sitting, squatting, kneeling on the affected knee or ascending and descending stairs.
On assessment:
- Swelling is often present immediately following acute trauma, however it can take up to 24 hours to appear clinically. The absence of an swelling does not necessarily rule out meniscal damage.
- Tenderness over the knee joint line will be evident when the knee bent to 45-90 degrees on either the inside or outside joint line depending on which meniscus is injured.
- Pain may be reproduced at full knee bend and straightening, which may be due to a torn meniscal flap or an effusion.
- There may be an inability to fully extend knee.
- Pain is usually present on deep squatting.
- A positive McMurray’s test (flexion/rotation test) is another common finding, and it involves the reproduction of pain and a “click or a clunk” on testing. Interestingly though, not all meniscus tears will exhibit a positive test. This is dependent on the size and type of the tear.
- MRI is a useful investigation that can add to the diagnosis and can help determine the location, size, and severity of the tear. This can be arranged by either the physio or GP when indicated. The finding of a meniscal tear on MRI does not necessarily mean that surgical intervention is required. Interestingly MRI found incidental meniscal tears in 60% of asymptomatic adults who were 60 years or older, (Hargrove, 2021), so it is important that we treat the patient and not just the patients scan results.

Treatment
If the injured patient does not report clicking or locking of the knee joint while moving, this is a good indication for conservative or “non-surgical” physiotherapy management of the knee. In the initial phase, physiotherapy management is aimed at regaining full extension of the knee to aid in normalised walking. This consists of manual therapy, load management, swelling management and exercise prescription to improve muscle activation of the quads, calf and glutes, flexibility exercises and gait retraining exercises.
Long term management looks at regaining the ability of the knee to tolerate higher loads (up/down stairs/hills, jogging) and control the knee through more dynamic movements (twisting/pivoting, changing directions, jumping and landing). This dynamic control is also known as proprioception—understanding where the knee is in space during movement.
Along the rehabilitation journey, load management (how much stress you put through your knee) is imperative to ensure that the knee does not undertake undue extra stress, which will cause further irritation to the meniscus, increasing swelling and potentially further tearing. Personal and lifestyle factors must be considered. These include:
- Job type—standing/sitting/manual labour
- Commute to work—public transport vs. driving (how far is the walk from parking spot)
- Family life—carer for family or dependents
- Daily incidental activities
- The differing demands of sport, hobbies and leisure activities
If the patient does report locking/catching of the knee or a trial of conservative physiotherapy management has not succeeded, this is an indication for surgical opinion and management. In this instance as physiotherapists we would liaise again with the patients doctor and organise for them to also see an orthopaedic surgeon who specialises in knees.
Surgical Management & Post-Op Rehabilitation
Surgical management can involve either a meniscal repair or an arthroscopic meniscectomy (removal of some or all the meniscus). A repair usually involves not moving the knee past 90 degrees of flexion for up to 6 months (usually guided by the surgeon), whereas after an arthroscope patient are often able to fully weight bear immediately and often start rehab immediately post-op. The process for rehabilitation after surgery is very similar to conservative management. Rehab is guided by the surgeon’s post-op protocol and can change if a meniscal repair occurs, however it usually follows the following phases.
Phase 1 aiming for pain and swelling control, return of full knee extension and quadriceps function. Passive knee flexion should be at 120 degrees by 4 weeks and we are aiming for normalised gait with minimal swelling.
Phase 2 is highly dependent on meeting key performance indicators rather than time: it involves regaining strength to > 70% strength of the unoperated limb, single leg balance for 30 seconds, ability to ascend/descend stairs without hip shift or pain. The patient is allowed to start low impact cardiovascular exercise.
Phase 3 includes strength training, multiplanar balance and stability and low intensity agility drills with predictable changes of direction. We aim to achieve > 80% strength in the surgical limb while re-introducing demand-specific athletic movement. (We are able to assess this using our AxIT strength Testing System.) As our patients progress through this phase of treatment, we typically rehabilitate them in a gym setting where we can prescribe and oversee agility drills, plyometrics and functional strength training.
Phase 4 includes return to sport training and > 90% strength in the surgical limb (Willsey, 2020) compared to the unaffected side.
What does the evidence say?
As mentioned earlier MRI found incidental meniscal tears in 60% of asymptomatic adults (people who had no pain or symptoms) who were 60 years or older (Hargrove, 2021), so it is important that we treat the patient and not just the patients scan results.
Herrlin (2011) found when comparing degenerative meniscal tears, patients that had arthroscopic surgery plus an exercise program had no additional benefit to an exercise program alone. This study validates that an exercise program compiled by a physiotherapist can be as effective as surgery. Brukner (2012) also suggests, that a physiotherapy approach should be undertaken for 3-4 weeks following meniscal tears, however as suggested earlier, failure with conservative management would require surgical intervention. By way of management the following table from Brukner & Khan (2012) outlines the typical evidence based approach.
Your content goes here. Edit or remove this text inline or in the module Content settings. You can also style every aspect of this content in the module Design settings and even apply custom CSS to this text in the module Advanced settings.
Conservative approach
|
· Symptoms develop 24-48 hours post injury · Minimal injury or unable to recall injury · Able to weight bear · Minimal swelling · Full ROM with pain only at end of range · Pain on McMurray’s test at end of range flexion only · Previous history of rapid recovery from similar injury · Early degenerative changes on x-ray |
Surgical Approach
|
· Severe twisting injury, unable to continue playing · Locked knee or severely restricted ROM · Positive McMurray’s test- “clunk” · Pain on early range flexion on McMurray’s test · Presence of ACL tear · Little improvement after 3-4 weeks of conservative treatment |
Brukner & Khan (2012)
The take home message.
Physiotherapy plays a big role in the rehabilitation of meniscal injuries as we help with both conservative management and post-op rehabilitation. If you are experiencing knee pain, and suspect that it might be a meniscal tear, then we suggest getting assessed by our physiotherapy team ASAP. The more urgently we see patients with meniscal pathology, the better chance of success with conservative “non-surgical” management as we help normalise their walking pattern and improve their muscle activation which typically leads to less pain, less dysfunction and a better outcome with an earlier return to function, life and sport.
Have you injured your knee and are concerned it could be your meniscus?
GET AN ASSESSMENT & TREATMENT WITH OUR AMAZING PHYSIO TEAM.
- Get a crystal clear diagnosis on what’s causing your pain or injury
- Understand what activities you can do without suffering further consequences of knee pain
- Commence rehabilitation improving your mobility and helping you get symptom free
- Set out a management plan so that you can achieve the best results
- Leave the session with the confidence of knowing exactly what to do to help you get pain free and back to sport, activity and full function